One of the key reasons we do not want to get diabetes is that we will be more likely to be hit by heart disease or stroke or even Alzheimer’s disease for that matter.
It’s scientifically proven. Having diabetes is associated with an increased risk of getting these disorders.
But, does diabetes cause heart diseases or stroke? Hmm, probably not.
Then what? Why are we more likely to get those diseases if we have diabetes?
The “ticking clock” hypothesis may provide the answer.
We are in the midst of a diabetes epidemic. Recent data suggests that 29.1 million people or 9.3 percent of the US population have diabetes. Among those, 28% are undiagnosed (1). Hence, 8.1 million people in the country have diabetes without knowing it.
Although the prevalence of both type 1 and type 2 diabetes continues to increase worldwide, type 2 diabetes is much more common, accounting for over 90 percent of patients with diabetes.
However, very few people die from diabetes itself. People die from the diseases that travel with it.
Cardiovascular disease is the leading cause of death in people with diabetes. Coronary heart disease accounts for more than 50 percent of all deaths while stroke accounts for approximately 15 percent (2).
Interestingly, there is evidence that the risk for coronary heart disease and stroke begins to increase long before the onset of clinical diabetes.
According to the “ticking clock” hypothesis, the clock for cardiovascular disease starts ticking many years before diabetes is diagnosed (3).
But how early in life can we see manifestations of heart disease? In fact, signs of cardiovascular disease are quite often found in early adulthood.
Atherosclerosis in Young People
In the 1950s, coronary heart disease was the most common cause of death in the industrialized world. The mounting epidemic had become a major threat to public health worldwide.
The underlying cause of coronary heart disease, atherosclerosis, is characterized by an accumulation of lipids, white blood cells (macrophages) and cell debris in the inner layers of the arterial wall. The process appears to be driven and maintained by chronic inflammation.

Although atherosclerosis can affect all arteries in the body, it has a specially strong affinity for the coronary arteries. The resulting thickening of the arterial wall and the building of plaques in the arteries may cause blockages and blood clotting to occur, subsequently damaging the heart muscle.
In 1953, a paper addressing the extent of atherosclerosis in young US soldiers killed in action in Korea was published (4). The results of the study were quite shocking.
Although the mean age of the soldiers was only 22 years, some evidence of atherosclerosis was found in 77 percent of the hearts.
The study had a profound impact on the awareness of the coronary heart disease epidemic and the existence of atherosclerosis in young, asymptomatic individuals.
So, it appears that atherosclerosis often starts at a young age, years before clinical symptoms of cardiovascular disease become manifest. The question is why the clock starts ticking. More recent studies have provided some clue.
In the late 1990s, a large autopsy study documented the frequent existence of atherosclerosis in young individuals without any symptoms of heart disease; most died as a result of trauma (5). Smokers and those with obesity or hypertension (high blood pressure) were most likely to have advanced atherosclerosis.
Hence, young people who smoke, are obese or have high blood pressure are more likely to have atherosclerosis at a young age.
The “Ticking Clock” Hypothesis
The San Antonio Heart Study, a population-based study of diabetes and cardiovascular disease conducted in the 1980s, was the first trial to seriously test the ticking clock hypothesis (3).
The investigators hypothesized that since individuals who are at risk of developing diabetes (prediabetes) have high levels of insulin (hyperinsulinemia), and since hyperinsulinemia is a risk factor for cardiovascular disease, prediabetic individuals might have a specific risk pattern even before the onset of clinical diabetes.
In the study, the cardiovascular risk factor status of 614 initially nondiabetic Mexican Americans who later participated in an 8-year follow-up of the San Antonio Heart Study was studied.
Individuals who were nondiabetic at the time of baseline examination, but who subsequently developed type 2 diabetes had higher levels of total and LDL cholesterol, triglyceride, fasting glucose, insulin, body mass index, and blood pressure, and lower levels of HDL cholesterol than subjects who remained nondiabetic.
Most of these differences persisted after adjustment for obesity and blood sugar level but were abolished after adjustment for fasting insulin concentration.
These results indicate that prediabetic subjects have an adverse risk factor pattern that may be present for many years and may contribute to the risk of cardiovascular disease as much as the duration of clinical diabetes itself. High insulin levels and insulin resistance, often present for years before diabetes develops, seem to play a key role.
The Nurses Health Study conducted in the 1970s, and 1980’s found that among women who developed diabetes during follow-up, the incidence of coronary heart disease was substantially elevated, both before and after diabetes was diagnosed, compared with women who remain free of diabetes (6).
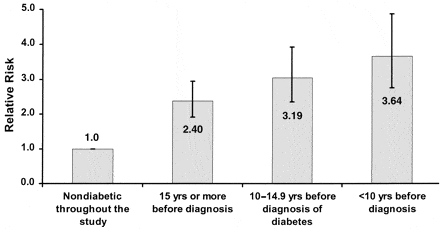
Consistent with the San Antonio Heart Study, the women who developed diabetes had a higher body mass index, and greater prevalence of hypertension and lipid abnormalities. However, the study findings suggest that the elevated cardiovascular risk before the diagnosis of diabetes can not be fully explained by the difference in conventional risk factors between non-diabetic and newly diabetic subjects.
The findings of both these studies provide support for the “ticking clock” hypothesis.
The “Common Soil” Hypothesis
Although controlling blood sugar plays a key role in the treatment of diabetes, good blood sugar control is not sufficient to avoid the development of diabetes-induced cardiovascular diseases. This suggests that factors not directly related to glucose metabolism may play a role.
Furthermore, the fact that the cardiovascular complications of diabetes seem to precede the onset of clinical diabetes suggests that rather than atherosclerosis being a consequence of diabetes, both conditions may have a common cause, i.e. they spring from a “common soil” (7). This is the “common soil” hypothesis.
A typical person at risk of developing diabetes has central obesity, high triglyceride levels, low HDL cholesterol, and high blood pressure. These are the main elements of the metabolic syndrome, and they are all associated with an increased risk of developing type 2 diabetes and cardiovascular disease. These individuals often have high insulin levels in their blood and show signs of insulin resistance.
Insulin resistance is defined as a diminished response to a given concentration of insulin. Initially, the pancreas responds by producing more insulin. However, as diabetes develops, the beta cells of the pancreas often become unable to produce more insulin, and its blood levels drop.
Individuals with insulin resistance and concomitant hyperinsulinemia are at risk of developing diabetes and cardiovascular disease.
Although insulin resistance is often associated with obesity, it is not present in all obese individuals. One study has suggested that the increased risk of cardiovascular disease associated with obesity may be confined to those with insulin resistance (8).
Whether the risk of cardiovascular disease associated with the metabolic syndrome is caused by the hyperinsulinemia and insulin resistance itself or other concomitant factors, such as central obesity, lipid abnormalities, and hypertension, remains controversial. Furthermore, other less obvious underlying factors may be important.
The metabolic syndrome is associated with elevated levels of inflammatory markers (9). Chronic low-grade inflammation is associated with increased risk of type 2 diabetes and heart disease (10).
Hence, inflammation might be an important link between cardiovascular diseases, insulin resistance, and the metabolic syndrome.
Endothelial dysfunction may also provide an important link between diabetes and heart disease.
The endothelium is a thin layer of cells that lines the interior surface of blood cells. These cells are in direct contact with the blood, and they are involved in the regulation of many functions of the vascular system.
It has been suggested that endothelial dysfunction and insulin resistance may synergistically increase the risk of cardiovascular disease in patients with type 2 diabetes (11).
Identifying People at Risk
The “ticking clock” hypothesis illustrates the importance of initiating preventive measures in people with diabetes long before diabetes becomes clinically manifest.
But how can we find those at risk? What do those who travel the road to diabetes and heart disease have in common?
Family history is important. Compared with people without a family history of type 2 diabetes, those with a family history in any first-degree relative have a two to three-fold increased risk of developing diabetes (12).
Central obesity, the accumulation of fat around the belly may be the first sign of increased risk. Central obesity is usually measured by waist circumference or waist-to-hip circumference ratio.
Impaired fasting glucose, impaired glucose tolerance, or a HbA1c level of 5.7 to 6.4 percent (39 to 46 mmol/mol) reflect abnormal glucose metabolism and are all associated with an increased risk of developing diabetes.
The triglyceride/HDL cholesterol ratio is associated with increased risk. One study found that a ratio above 4 was a powerful independent predictor of developing coronary artery disease (13).
Although LDL cholesterol is often used to assess the risk of future cardiovascular events, many patients with the metabolic syndrome have normal or close to normal values. Thus, relying on LDL cholesterol in this population may be misleading.
Although predicting the risk of cardiovascular events by a clinical risk score using conventional risk factors is common practice, it may be dreadfully misleading in the clinical setting.
Recent studies have shown that coronary calcium score (assessed by CT scan) may be very helpful to predict risk (14). A coronary calcium score of zero confers a 15-year warranty period against mortality in individuals at low to intermediate risk that is unaffected by age or sex.
Reducing Risk
How can those who run the risk of developing diabetes and cardiovascular disease reduce their risk?
Many of these individuals have general or central obesity and will benefit from weight loss.
Refraining from smoking is immensely important. In a meta-analysis of 25 prospective cohort studies, current smokers had an increased risk of developing type 2 diabetes compared with nonsmokers (15). Furthermore, smoking is a strong risk factor for coronary heart disease and stroke.

Regular exercise is helpful.
Studies have shown that sedentary lifestyle increases the risk of diabetes (16). Moderate physical activity, including brisk walking, is associated with a lower risk of developing diabetes compared with being sedentary (17).
Diet
Interestingly, there are very few trials that have examined the effects of diet alone for the prevention of diabetes (18).
A low-fat dietary pattern among generally healthy postmenopausal women showed no evidence of reducing diabetes risk after 8.1 years in the Women’s Health Initiative Dietary Modification Trial which studied 48,000 postmenopausal women. (19).
A meta-analysis of epidemiological studies and clinical trials on the metabolic syndrome showed that adherence to the Mediterranean dietary pattern was beneficial (20). Waist circumference, HDL cholesterol levels, triglyceride levels, blood pressure levels, and glucose metabolism were all positively affected.
One study addressing individuals with the metabolic syndrome compared a Mediterranean diet with a prudent low-fat, high carbohydrate diet. Individuals on the Mediterranean diet showed signs of less inflammation, less insulin resistance and less endothelial dysfunction(21).
There is now convincing evidence that increased intake of sugar-sweetened beverages increases the risk for metabolic syndrome, type 2 diabetes, coronary heart disease, and stroke (22,23).
Therefore, avoiding added sugar and refined carbohydrates is of key importance for those at risk of diabetes and cardiovascular disease.
Furthermore, several studies suggest that carbohydrate restriction has more favorable effects on the metabolic syndrome than a low-fat diet (24, 25, 26,27, 28). Low-carbohydrate diets tend to lead to more weight loss, less insulin resistance, lower triglyceride levels, and higher levels of HDL-cholesterol.
Statin drugs
Statin drugs are recommended for people at increased risk for cardiovascular disease and those with diabetes.
It has been assumed that statins reduce cardiovascular risk in patients with the metabolic syndrome by alterations in lipid levels and possibly by decreasing inflammation (29).
However, the clinical efficacy of statin therapy has not been specifically tested or compared to lifestyle modification in people with prediabetes or the metabolic syndrome.
In fact, statins may be a double-edged sword in this population as they have been shown to increase the risk of diabetes. A recent Finnish study of men with metabolic syndrome suggests that the risk of statin-induced diabetes may be higher than previously reported (30).
The Bottom-Line
People usually don’t die from diabetes. Most diabetics die from diseases that travel with their diabetes, such as heart disease or stroke.
According to the “ticking clock” hypothesis, the increased risk of cardiovascular disease associated with type 2 diabetes is already present years before diabetes is diagnosed.
The hypothesis suggests that factors other than diabetes itself may contribute to the risk of cardiovascular disease among diabetics.
Therefore, preventive measures aimed at reducing risk among the rapidly growing population of people with type 2 diabetes will have to be initiated long before diabetes becomes manifest.
Weight loss, regular exercise, not smoking and treatment of high blood pressure are all important measures that may reduce risk.
Carbohydrate restriction and a Mediterranean-type diet can improve many of the features associated with increased risk of cardiovascular disease among people at risk of developing diabetes.
Avoiding added sugar and refined carbohydrates are of key importance.


Typo – How can those (how) run the risk of developing diabetes and cardiovascular disease reduce their risk?
Recently published research suggests that low-fat dairy consumption may have contributed to the diabetes epidemic. “Interestingly, despite widespread recommendations for consumers to avoid high fat foods (including whole fat dairy products), previous studies in humans have demonstrated that whole fat dairy consumption is associated with multiple health benefits, including lower risks of insulin resistance, metabolic syndrome, and type 2 diabetes.” https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0132117
And some yet to be published research connects high soybean oil intake to diabetes. “A diet high in soybean oil causes more obesity and diabetes than a diet high in fructose, a sugar commonly found in soda and processed foods, according to a new study. In the U.S. the consumption of soybean oil has increased greatly in the last four decades due to a number of factors, including results from studies in the 1960s that found a positive correlation between saturated fatty acids and the risk of cardiovascular disease.” https://www.sciencedaily.com/releases/2015/07/150722144640.htm
A study conducted among dolphins? Please. Might be relevant if you’re planning to grow a pair of fins anytime soon 🙂
Seriously David, you’ve got it backwards: low fat dairy is associated with a DECREASED risk. See e.g.
https://www.health.gov/dietaryguidelines/dga2015/comments/uploads/CID813_AJCN_Editorial_SFA_Astrup.pdf
Are there any studies done on anything in the absence or minimization of carbs? I am having a hard time finding a truly low carb high fat ketogenic study. I agree that fats in the presence of carbs are bad, but who is really the bad guy? Any studies out there that involve homosapiens?
I didn’t state that fats & carbs together are bad. If you’re talking about the Western Diet (junk food = high in sugar & trans & sat. fats), then I agree.
I know you didn’t state carbs and fats together are bad, I did. I am a type 2 diabetic, I have found no good carbs that allows me to control my BG. I have also found no studies of a diet that included very low carbs and fats, healthy natural saturated fats, and they are always pointed at as being the villain. I want to see something that separates the carbs out and proves its the fats.
What do you mean by the last sentence? And what are “natural saturated fats”?
All the high fat studies I have seen contain a majority of carbs in the diet. I would like to see a study that was truly a ketogenic diet and its impact on heart diseases. You know of one or more?
Saturated fats that occur naturally in foods, animal and plant.
No studies with hard end points, that’s true. And yes, all the longer studies include diets which aren’t ketogenic.
For the latter part: ok. Although safas in foods aren’t healthy, neutral in some contexts.
mbuster
Take a look at references 24, 25, 26,27 and 28 in the paper above
I’m not seeing the detail I’m looking for in terms of cardiovascular risks. Already aware of weight loss benefits with n=1. My main concern of n=1, i had recent quad bypass and wanting to avoid future event. Concern is did going LCHF set off or delay blockages found, I was asymptomatic. I was told it didn’t happen overnight, and most probably genetics. I’m not convinced that the term genetics is not loosely misinterpreted as the effects of major nutritional guideline changes occurring in the 1950-70s.
Closest thing seems to be 27 with closing comment of ” Future studies evaluating long-term cardiovascular outcomes are needed before a carbohydrate-restricted diet can be endorsed.”
I’m not aware of any randomized study study with hard clinical endpoints that has compared low carb vs. low fat.We only have data on surrogate endpoints (lipids, BMI, blood pressure, inflammatory markers etc).
With regards to hard cardiovascular end points you’ll find most data on the Mediterranean diet and most of the data is in favour of that dietary approach.
Thank you, Dr. Sigurdsson, for your response. I will start leaning in that direction of curiosity with a cause.
Don’t know why I didn’t catch this when I first read it, but it sure prompts a relevant question for me, have you already written or can you write in the future on inflammatory markers? How does diet specifically increase/decrease them?
I did write an article a while back on diet and inflammation https://www.docsopinion.com/2013/08/20/top-10-things-you-should-know-about-diet-and-inflammation/
You’re right. There’s no study with hard clinical endpoints that has compared low carb vs. low fat.We only have data on surrogate endpoints (lipids, BMI, blood pressure, inflammatory markers etc).
With regards to diet and studies with hard cardiovascular end points you’ll find most data on the Mediterranean diet and most of the data is in favour of that dietary approach.
Mie
Interesting conclusion from the editorial you cited: “There is no evidence left to support the existing public health advice to limit consumption of dairy to prevent CVD and type 2 diabetes. Cheese and other dairy products are, in fact, nutrientdense foods that give many people pleasure in their daily meals”
There is an inverse association between consumption of dairy products and the metabolic syndrome in overweight, but not lean adults.
In the Coronary Artery Risk Development in Young Adults (CARDIA) study, overweight subjects with the highest consumption of dairy products had a significantly lower risk of the metabolic syndrome as compared with those with the lowest dairy consumption https://www.ncbi.nlm.nih.gov/pubmed/11966382.
In other prospective studies, low-fat, but not high-fat dairy intake, was associated with a lower risk of type 2 diabetes (independent of BMI)
https://www.ncbi.nlm.nih.gov/pubmed/15883237 https://www.ncbi.nlm.nih.gov/pubmed/16801582
Yes, the conclusion is … “interesting”. Or rather misguided in the sense that full-fat dairy products seem to be neutral at best. In other words, if you’re a high-risk individual, you’re better off using low-fat dairy products which seem to be beneficial and LOWER the risk (unlike full-fat dairy products).
Mie
But, as I said, the situation appears different if you’re overweight. Then the intake of high-fat dairy products is associated with lower risk (CARDIA study).
But all in all, the risk for IRS was smaller for reduced fat dairy products (see table 5). When looking at individual components, high fat was superior in some cases and low fat in other cases.
In addition, unless there’s more than one cohort study to back up the claim, I wouldn’t root for high-fat dairy for the obese.
Instead of your one study that came up with the Mediterranean diet (ref 20), which was published in 2004, how about looking at this one, which was published a few years later, and compared three diets? The low carb diet came out a winner: https://www.ncbi.nlm.nih.gov/pubmed/18635428
Thanks Emm deWorde
I also referred to a meta-analysis of 50 studies on the effect of Mediterranean diet on metabolic syndrome and its components, published 2011 (ref 19)
What do you mean by “winner”? The trial assessed the issue of weight loss, not hard end points relevant to the matter at hand (CVD/diabetes).
As I have previously noted, since most docs seem to usually classify diabetes as a relatively minor risk for statin use, I wonder if the risk factors and overall mortality risk associated with statins might be significantly underestimated, since I suspect that statin use is not commonly linked to diabetes related serious medical problems and deaths.
I was struck by the similarities between the Finnish study on statins & diabetes that you noted (also discussed below) and the nurses study on the same topic:
Statins Raise Diabetes Risk In Post-Menopausal Females
https://www.medicalnewstoday.com/articles/240148.php
Statins Linked to Raised Risk of Type 2 Diabetes (White males age 45 to 73)
https://www.webmd.com/diabetes/news/20150304/statins-linked-to-raised-risk-of-type-2-diabetes
A link to and an excerpt from a WSJ article which discusses recent research that the TG/HDL Ratio is the most accurate predictor of early arterial damage in children and young people. As noted in the article, due to young people’s tendency to have lower TG levels, the doc quoted in the article would be concerned if a younger patient has a TG/HDL Ratio over 2.7 (US metrics).
WSJ: Children on Track for a Heart Attack
https://www.wsj.com/articles/SB10001424127887323798104578453123376765286
Excerpt:
There has been much discussion of the following article, but a question I have had for a while is why did the researchers not look at the TG/HDL Ratio for the large group of patients, since they had separate TG and HDL charts? Is there any way to access the data and show the TG/HDL Ratios for the group of 136,905 patients hospitalized with coronary artery disease?
Lipid levels in patients hospitalized with coronary artery disease: an analysis of 136,905 hospitalizations in Get With The Guidelines.
https://www.ncbi.nlm.nih.gov/pubmed/19081406
And why don’t we look at the number of patients with LDL 60 irregardless of LDL. Why conclude lowering of LDL is beneficial along with the raising of HDL with that information excluded. Yes, I already preconceive that higher HDL is beneficial.
I also make an article about this disease. thank you so much want to share this information. very helpful at all.
Visit: obat luka gangren