Estimated reading time: 10 minutes
Fish oil is one of the most commonly used dietary supplement.
It has been recommended by some major societies and public health authorities for cardiovascular risk modification, to treat high blood triglycerides and as a treatment following acute myocardial infarction (heart attack).

However, many questions remain unanswered. How does fish oil improve health? Is the evidence strong enough to recommend its use? Should it be recommended to everyone or only those at increased risk of heart disease? Are there any side effects? What’s the optimal daily dose? Is consuming oily fish enough or do we need additional fish oil supplement?
History
More than forty years ago, Danish scientists found that the total amount of fat in the diet of Americans, Danes and Greenland Eskimos was similar (1).
At the same time they reported that the death rate from coronary artery was much lower among the Greenland Eskimos, compared with the Americans and Danes.
While visiting Greenland and studying the diet of the native Eskimos, the Danish researchers found that their diet was indeed quite different from that in the US and Denmark.
The fat content of the native diet was largely from whale blubber, seal fat, and fish fat, all very high in omega-3 fatty acids.
The scientists attributed the low death rate from heart disease among the Eskimos to the high consumption of marine-derived omega-3 fatty acids.
Recently, a Canadian paper (2) claimed that the Danish researchers may have underestimated the incidence of coronary artery disease among the Inuits, and therefore their conclusions may not be valid. However, these early studies sparked a great amount of interest among scientists in the possible cardiovascular benefits of omega-3 fatty acids.
Since then, scientific studies have have identified two types of long chain omega-3 polyunsaturated fatty acids in fish oils as the most likely active constituents behind the positive health effects of seafood. These are eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA).
Omega-3 Fatty Acids
The body can synthesize most fatty acids as it needs them. Therefore, it is not necessary to get them in the diet.
Some fatty acids cannot be produced by the human body. This is true for the omega-6 and omega-3 fatty acids. These fatty acids must come from food and are therefore called essential fatty acids.
Omega-3 fatty acids are polyunsaturated fatty acids with a double bond at the third carbon atom from the end of the carbon chain. There are three main types; alpha-linolenic acid (ALA), EPA and DHA. ALA is found in many vegetable oils (rapeseed, flaxseed, and soybean), seeds and nuts. EPA and DHA are typically found in fatty fish and fish oils.
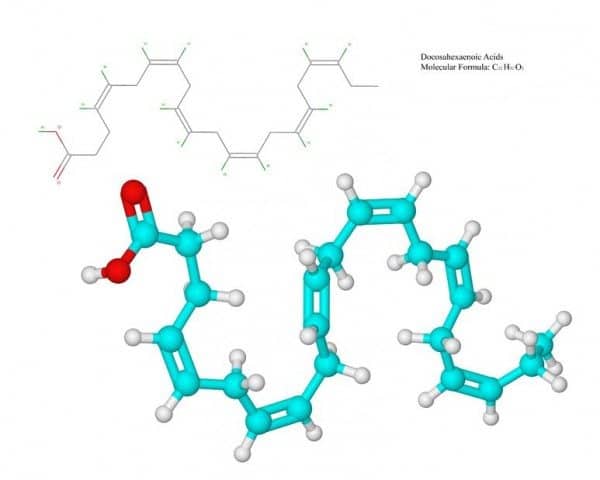
ALA is an 18-carbon fatty acid with three double bonds (18:3). It can be elongated and desaturated in the body to EPA with 20 carbon atoms and five double bonds (20:5) and DHA with 22 carbons and six double bonds (22:6).
However, for these reactions to occur it must compete with omega-6, so only a fraction of ALA is converted to EPA and DHA.
Like other dietary fatty acids, EPA and DHA are transported in the circulation mainly as triglycerides in lipoprotein particles. These two fatty acids are incorporated into phospholipids in cell membranes throughout the body, particularly in the heart and brain. They are also stored in fat tissue as triglycerides.
The Effects of Fish Oil on Health and Cardiovascular Disease Mechanisms
The intake of marine omega-3 fatty acids may have several health benefits. For example, some studies suggest positive effects on rheumatoid arthritis (3), inflammatory bowel disease (4) and Alzheimer’s disease (5). There is also evidence suggesting that fish oil may promote hair growth (6).
Most of the research on the possible health benefits of omega-3 fatty acids has been within the field of cardiovascular medicine. Several studies have addressed the effects on cardiovascular risk factors, endothelial function, blood clotting and inflammation.
Fish Oil and Blood Lipids
High blood levels of triglycerides, LDL cholesterol (the bad cholesterol) and low levels of HDL cholesterol (the good cholesterol) are associated with increased risk of heart disease.
Intake of fish oil can lower blood levels of triglycerides by as much as 50 percent (7). Relatively high doses are needed to achieve this effect (up to 3-4 g/day).
Fish oil consumption modestly elevates blood levels of LDL cholesterol and HDL cholesterol.
Intake of omega-3 may lower the preponderance of small dense LDL-particles (8). This may account for the slightly raised LDL cholesterol. Large particles can carry more cholesterol. However, small LDL-particles have a stronger association with cardiovascular risk than large particles (9).
Fish Oil, Blood Pressure and Heart Rate
High blood pressure is a risk factor for coronary artery disease, heart failure and stroke.
Many studies have addressed the effects of fish oil on blood pressure. A meta-analysis of 36 randomized trials (10) indicated that fish oils may reduce both systolic and diastolic blood pressure, especially among elderly people with hypertension. Relatively high doses were used in most of these studies (median dose 3.7 g/d).
It is believed that the blood pressure lowering effects of fish oil is due to reduced vascular resistance in small arteries, probably mediated by increased production of nitric oxide. Nitric oxide is a powerful vasodilator (dilates arteries).
Studies also suggest that intake of fish oil lowers heart rate (11).
Fish Oil and Endothelial Function
The endothelium is a thin cellular layer lining the innermost part of the arteries. Endothelial cells are in direct contact with circulating blood. The endothelium plays an important role for the regulation of blood flow.
Abnormal endothelial function is often found among people with high blood pressure, diabetes and heart disease. Improving endothelial function may be important for individuals suffering from these disorders.
Several randomized studies have suggested that fish oil improves endothelial function (12).
This effect may explain some of the proposed beneficial effects of omega-3 fatty acids on cardiovascular function.
Fish Oil and Blood Clotting
During the early studies of the dietary habits and health of the Inuits it became apparent that they often suffered from nose bleeds. This is probably due to the increased bleeding time caused by ingestion of high doses of omega-3 fatty acids.
Despite the increased bleeding time, clinical studies have not shown that high doses of omega-3 fatty acids increase the rates of clinical bleeding problems (13).
Whether fish oils can reduce the risk of thrombosis (blood clotting inside blood vessels) remains to be proven.
Fish Oil and Inflammation
EPA and DHA are precursors to substances called eicosanoids. Eicosanoids are important regulators of inflammation.
Therefore, many experts believe that fish oils may help to reduce chronic low-grade inflammation.
Although some studies have not been able to show that fish oil consumption reduces blood markers of inflammation, other studies (14) have suggested that they may do so when relatively high doses are given (> 2 g/day).
Clinical Efficacy of Fish Oil
The clinical efficacy of fish oil has been intensively studied, particularly in the field of cardiovascular disease. A number of trials haves assessed the effects on coronary heart disease, arrhythmia (heart rhythm disorders) and sudden death.
Many experts believe that the positive effects of fish oil consumption on blood lipids, blood pressure, endothelial function, blood clotting and inflammation may be translated into improved clinical outcome.
There are three important questions that have to be asked about the efficacy of fish oils when it comes to cardiovascular disease. Firstly, does intake of fish oils lower the risk of healthy individuals. Secondly, does fish oil reduce risk among people at increased risk. And finally, does fish oil consumption improve outcome among these already affected by heart disease?
So, what do the studies say?
Fish Oil and Coronary Artery Disease
Observational studies on the consumption of fish and fish oils among western populations have shown conflicting results.While some studies have indicated less risk of cardiovascular disease among individuals with high consumption of fish and fish oils, others have not (15, 16).
In a large Japanese cohort, where the intake of omega-3 fatty acids was high, consumption of fish and fish oils was associated with reduced risk of coronary heart disease (17).
One systematic review and meta-analysis pooled data from 19 large prospective cohort studies and randomized trials in participants consuming either fish or fish oil supplements. The study found that consumption of marine omega-3 fatty acids was associated with lower risk of death from heart disease and sudden cardiac death (18). The authors concluded that the benefits of fish consumption exceed the potential risks.
Randomized clinical trials have studied whether fish oil intake may reduce the risk of cardiovascular events. Some of these studies have indicated a positive effect while others have not.
One of the first randomized trials addressing the issue was published in 1989 (19). Two groups of more than 1000 men each who had just had a myocardial infarction (heart attack) were studied. One group was advised to ingest oily fish two times a week. The other group was not given this advice. After two years, there was a 29% reduction in life-threatening arrhythmias in the men advised to eat oily fish compared with the other group.
These initial results were later supported by the GIZZI-Prevenzione Trial (20), a large prospective randomized trial of more than 11.000 patients who had a recent myocardial infarction. Compared with placebo, 850 mg EPA+DHA significantly lowered the risk of death due to cardiovascular causes as well as death from all causes. There was a 45 % reduction in the risk of sudden death.
However, these highly positive results were not replicated in subsequently published large trials (21, 22, 23).
A meta-analysis of available randomized clinical trials published 2012 indicated that omega-3 fatty acid supplementation was not associated with a lower risk of heart attack or stroke or death from any cause, death from heart disease or sudden death (24).
The large Risk and Prevention Study, a double-blind placebo controlled trial published 2013 enrolled 13.513 patients with multiple cardiovascular risk factors or known cardiovascular disease (24). Patients were assigned 1 g/day of omega-3 fatty acids or placebo (olive oil). After a median follow–up of five years, the number of cardiovascular deaths, heart attacks and stroke was similar in both groups.
In this study, the participants received maximal medical therapy including aspirin, angiotensin-converting enzyme (ACE) inhibitors, beta-blockers and cholesterol-lowering drugs. It has been suggested that the beneficial effects of omega-3 fatty acids may be diminished in patients already receiving aggressive risk management.
Administration and Dosing
EPA and DHA are found in cold-water fish such as salmon, mackerel, halibut, sardines, tuna, and herring.
Many over-the-counter preparations of fish oil are available. There is also a prescription formula (Lovaza, Omacor) in the US.
Different fish oil formulations contain variable amounts of EPA and DHA. Thus, a 1 g capsule may contain between 200 and 950 mg of EPA and DHA. A common amount in fish oil capsules is 180 mg of EPA and 120 mg of DHA, a total of 300 mg (EPA + DHA).
It is believed that a reasonable target intake to affect cardiovascular risk is 250 to 500 mg/day of EPA + DHA. This can be achieved by 1 g/day of fish oil supplement (between 200 to 800 mg of EPA+DHA, depending on the formulation) or 1-2 servings per week of fatty fish.
Although it appears that higher doses are safe, the US FDA does not recommend ordinary daily intakes of more than 2 g EPA+DHA. However, doses of 4 g/day have been approved for the treatment of high blood triglycerides (hypertriglyceridemia).
Fish Oils and Cardiovascular Disease – The Bottom Line
Treatment with marine-derived omega-3 fatty acid for the prevention of major cardiovascular adverse outcomes is supported by a number of randomized clinical trials and refuted by others.
Therefore, it is hard to give general advice on fish oil as a tool to reduce the risk of cardiovascular events among healthy people or to improve prognosis among those already affected by cardiovascular disease.
We will have to await results from ongoing clinical trials to further clarify this issue.

Here’s a strong video argument from Dr. Michael Greger that fish oil is increasing inflammation markers, rather than shrinking them. He attributes this to the high loads of industrial pollutants that are contaminating even the so-called purified fish oils (which are largely unregulated). He recommends that anyone who wants to consume fish oil should use the algae-based products instead.
https://nutritionfacts.org/video/is-distilled-fish-oil-toxin-free/
Russel. Thanks for the tip. Will take a closer look at the issue.
Yes, markers, not hard end points. Based on a single study with healthy subjects which means the results can HARDLY be extrapolated to e.g. heart disease patients. Greger’s vegan bias strikes again.
As for studies like this
https://www.nejm.org/doi/full/10.1056/NEJMoa1205409
you’d be wise bear in mind that a) the placebo comparison itself (olive oil) is a healthy choice which obviously attenuates the findings and b) the amount of fish oil was much, much more modest than in studies where the greatest benefits have been shown (e.g. GIZZI). And, just like Axel mentioned, when discussing patients already on an aggressive lipid-lowering etc. etc. treatment, the benefits are naturally going to be more modest.
I agree with Axel on fish oil not being a magical cure for all & everyone, but for those at risk of CHD and who cannot eat fish, fish oil supplementation is worth considering.
I know it is outside your area of expertise but why no mention of the effect of omega-3’s in suppressing the immune system?
https://www.ncbi.nlm.nih.gov/pubmed/1833105
https://mpkb.org/home/othertreatments/efas
Neil.
Thanks for highlighting the possible immuno-suppresive effects of omega-3. Interesting.
Hopefully future research will tell us more about this and what it means in terms of clinical relevance.
Purified fish oil is a supplement. Unfortunately, no amount of supplementation can negate the effects of excessive omega-6 linoleic acid (LA) intake. Excerpt from page 191 of “The Modern Nutritional Diseases: And How to Prevent Them” by Fred and Alice Ottoboni.
“BIOCHEMICAL LESSON: The significant point is that good health depends on regulating the D5D enzyme. High insulin levels due to dietary sugar and starch and high dietary omega-6 to omega-3 ratios, stimulate the D5D enzyme, and move the biochemical set point from normal toward inflammation. On the other hand, control of dietary sugar and starch, reduction of LA in the diet, and a daily supplement of fish oil to provide EPA will inhibit the D5D enzyme so that the appropriate amounts of both proinflammatory and anti-inflammatory eicosanoids are produced. Keep in mind that all of the eicosanoids, both the so-called good and bad, are important. The body is designed to use eicosanoids with opposing effects to control vital functions. In a state of optimum health, the good and the bad eicosanoids balance one another.”
You almost never see a recommendation to reduce LA intake. It’s always about increasing omega-3 fish oil to balance omega-6 to omega-3 ratios. This is especially strange in light of this research:
Commentary: “Human intelligence has a physical basis in the huge size of our brains. It is some seven times larger than would be expected for a mammal with our body size,” said Steven Gaulin, UCSB professor of anthropology and co-author of the paper. “Since there is never a free lunch, those big brains need lots of extra building materials. Most importantly, they need omega-3 fatty acids, especially DHA. Omega-6 fats, however, undermine the effects of DHA and seem to be bad for brains.” https://www.designntrend.com/articles/19655/20140916/fats-breast-milk-linked-academic-success.htm
Research: ” The fatty acid contents of human milk samples from 28 countries were used to predict averaged 2009 and 2012 test scores in mathematics, reading, and science from the Program for International Student Assessment. All test scores were positively related to milk docosahexaenoic acid, and negatively related to linoleic acid. https://www.ncbi.nlm.nih.gov/pubmed/25172360
High omega-6 intake prior to pregnancy also affects the intelligence of offspring. During the third trimester of pregnancy, the mother’s body obtains fats from fat stores to build brain tissue. If fat stores are rich in omega-6s and deficient in omega-3s the baby gets an inferior brain. https://www.anth.ucsb.edu/sites/secure.lsit.ucsb.edu.anth.d7/files/sitefiles/people/gaulin/n-3%20cog_frontiers.pdf
Hello Doc. I just received my results and HDL/Trig Ratio is 1.2. However, LDL-P is 2500. I’m on High sat fat diet which I think has hiked those numbers up. I don;t have thyroid issues (checked) and now looking at possible leaky gut/toxemia. My hsCRP is 1, so I really have no idea what is going on. Any thoughts..?
Thanks for this post!
I’ve read quite a bit about supplements. We do take fish oil and get about 2 gm/day along with magnesium, multivitamins.
This is the most thorough summary of research and dosing of fish oil I’ve ever seen.
Thanks. Glad you appreciate it.
Awesome post. My online dietitian suggested me to take fish oil as supplement. Consult a dietitian always when you are trying something new for your health like dieting, exercise etc. Get online tips from a dietitian 24/7 at eVaidya. https://www.evaidya.com/home.html#!/staticDoctors/Name/Language/Location/Dietician-or-Nutritionist
Hi Doctor Sigurdsson,
Many thanks for your message regarding the NNT and thanks for your blessings 🙂
This is a great article on fish oil.
As of today, in your opinion, will taking a fish oil supplement in capsules help to lower risks in patients who never had MI ? (assuming taking a 5 star IFOS rating high quality purified fish oil supplement in capsules)
Many studies used a fish oil supplemental dosage of 1800 mg of EPA + DHA per day to stabilize plaque, slow the progression of stenosis and lower inflammatory markers. Do you think 1800 mg of EPA + DHA per day is the optimal dosage?
In humans, will taking 1800 mg of EPA + DHA per day cause the LDL particles more prone to oxidation in vivo? (as EPA & DHA can easily go rancid, once they are incorporated into the membrane of the LDL particles, the LDL particles become rancid as well)
If so, will taking ubiquinol supplements help to mitigate the LDL oxidation?
Many thanks for your ideas 🙂
Cheers,
Quin
Hi Doctor Sigurdsson,
Can you please share some ideas? many thanks 🙂