Estimated reading time: 13 minutes
Stomach pain, also known as abdominal pain, is caused by a variety of conditions most of whom are innocent or benign.
However, sometimes, abdominal pain may be due to a severe disorder needing immediate intervention.
The abdomen is the part of the body between the chest and the pelvis. Other common names used to describe the abdomen are belly, stomach, and tummy.
The location of the pain is a of key importance. Hence, pain may be classified as upper abdominal pain and lower abdominal pain.
Upper abdominal pain is further divided into upper right abdominal pain, epigastric pain, and upper left abdominal pain.
Lower abdominal pain may also be divided into right and left lower quadrant pain.
Abdominal pain can also be diffuse and not distinctly positioned in a particular part of the abdomen.
Acute vs. Chronic Abdominal Pain
Determining whether the pain is acute or chronic is crucial.
The term ‘acute abdomen’ was defined to describe a rapid onset of severe abdominal pain that may represent a serious condition. It needs an urgent and specific diagnosis and sometimes immediate surgical intervention.
Examples of underlying causes of ‘acute abdomen’ are acute appendicitis, acute cholecystitis, acute pancreatitis, acute diverticulitis, gallstones, and kidney stones.
Upper Right Abdominal Pain
Upper right abdominal pain is typically caused by disorders of the liver, gallbladder, and biliary tree.
1. Gallstones
Pain caused by gallstones is called biliary colic.
Biliary colic is a steady or intermittent ache usually located in the upper right abdomen. Sometimes the pain spreads backward to the right shoulder blade.
The pain usually lasts for 30 minutes to an hour but may continue at a lower intensity for several more hours.
Ultrasound is commonly used to detect gallstones.
Surgical removal of the gallbladder is a standard treatment for patients with gallstones and biliary colic. It is often performed by keyhole (laparoscopic) surgery.
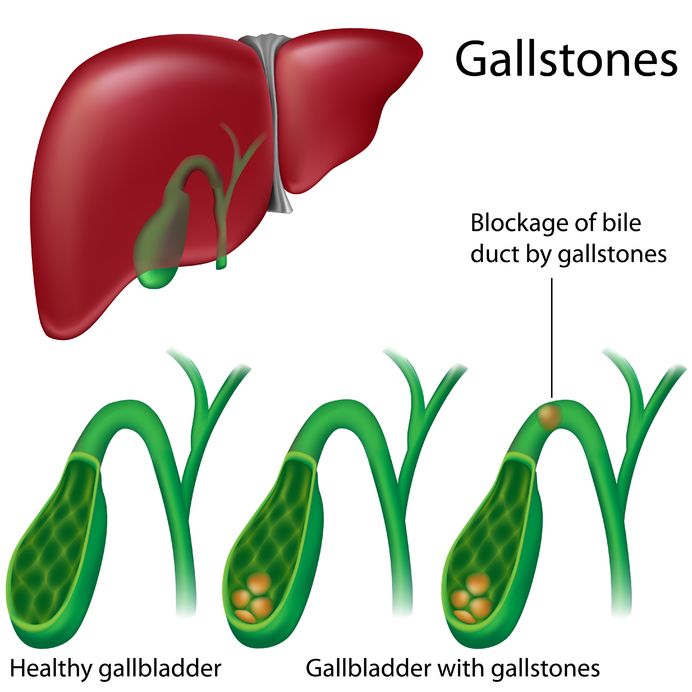
2. Acute Cholecystitis
Acute cholecystitis is an inflammation of the gallbladder.
Gallstones blocking the transport of bile from the gallbladder are the most common underlying cause.
Most often, patients experience steady, severe upper right abdominal pain. Nausea and vomiting are common and fever is usually present as well.
Hospital admission is usually necessary.
Treatment is based on fasting, pain medication, and antibiotics if an infection is present.
Sometimes, removal of the gallbladder is necessary.
3. Acute Cholangitis
Acute cholangitis is caused by a bacterial infection of the bile ducts. It occurs when gallstones become impacted in the biliary ducts (1).
Sometimes, a tumor blocking the bile ducts is the underlying cause.
Acute cholangitis is characterized by fever, jaundice, and abdominal pain (2).
Jaundice is a term used to describe yellowing of the skin and the whites of the eyes. It is caused by the build-up of a substance called bilirubin in the blood and tissues of the body.
Cholangitis is a serious medical condition.
Treatment includes fasting and intravenous fluids.
Antibiotics are administered to treat the underlying infection.
It is essential to restore normal flow in the bile ducts by removing the blockage.
4. Hepatitis
Hepatitis is an inflammation of the liver, usually caused by a viral infection.
Typical symptoms include right upper right abdominal pain, fatigue, nausea, vomiting, and clay-colored stools. Furthermore, some patients have dark urine and jaundice as well.
There are several types of viral hepatitis.
Hepatitis A is caused by the hepatitis A virus. The virus is primarily spread when a person ingests food or water that is contaminated with the feces of an infected person. The disease is closely associated with unsafe water or food, inadequate sanitation, and poor personal hygiene (3).
Hepatitis B is also caused by a viral infection. The virus is transmitted through contact with the blood or other body fluids of an infected person.
The disease may lead to scarring of the liver. Moreover, there is an increased risk of liver cancer and liver failure.
Most patients with hepatitis B have no symptoms.
A vaccine is available for both hepatitis A and B.
Hepatitis C is caused by the hepatitis C virus. It is a blood-borne virus and usually spreads through exposure to small quantities of blood. This commonly happens through injection drug use.
Approximately 80% of people with hepatitis C have no symptoms.
Some patients have mild symptoms but others suffer from a serious, lifelong illness (4).
A significant number of those who are chronically infected will develop scarring of the liver or liver cancer (5).
Medical treatment for hepatitis C is available but remains limited.
Epigastric pain
Epigastric pain is located in the central portion of the upper abdomen, below the sternum, and above the navel. It is often caused by disorders of the stomach and pancreas.
Dyspepsia is a common term used to describe epigastrial pain, sometimes combined with other complaints (6).
5. Peptic Ulcer Disease (PUD)
Ulcers in the lower esophagus, the stomach, and the first part of the small intestine (duodenum) are common causes of epigastrial pain. Together these disorders are known as peptic ulcer disease (PUD).
PUD is characterized by a gnawing or burning sensation in the epigastrium (7).
Infection of the lining of the stomach from a bacteria called H pylori is a common underlying cause of peptic ulcer disease (8).
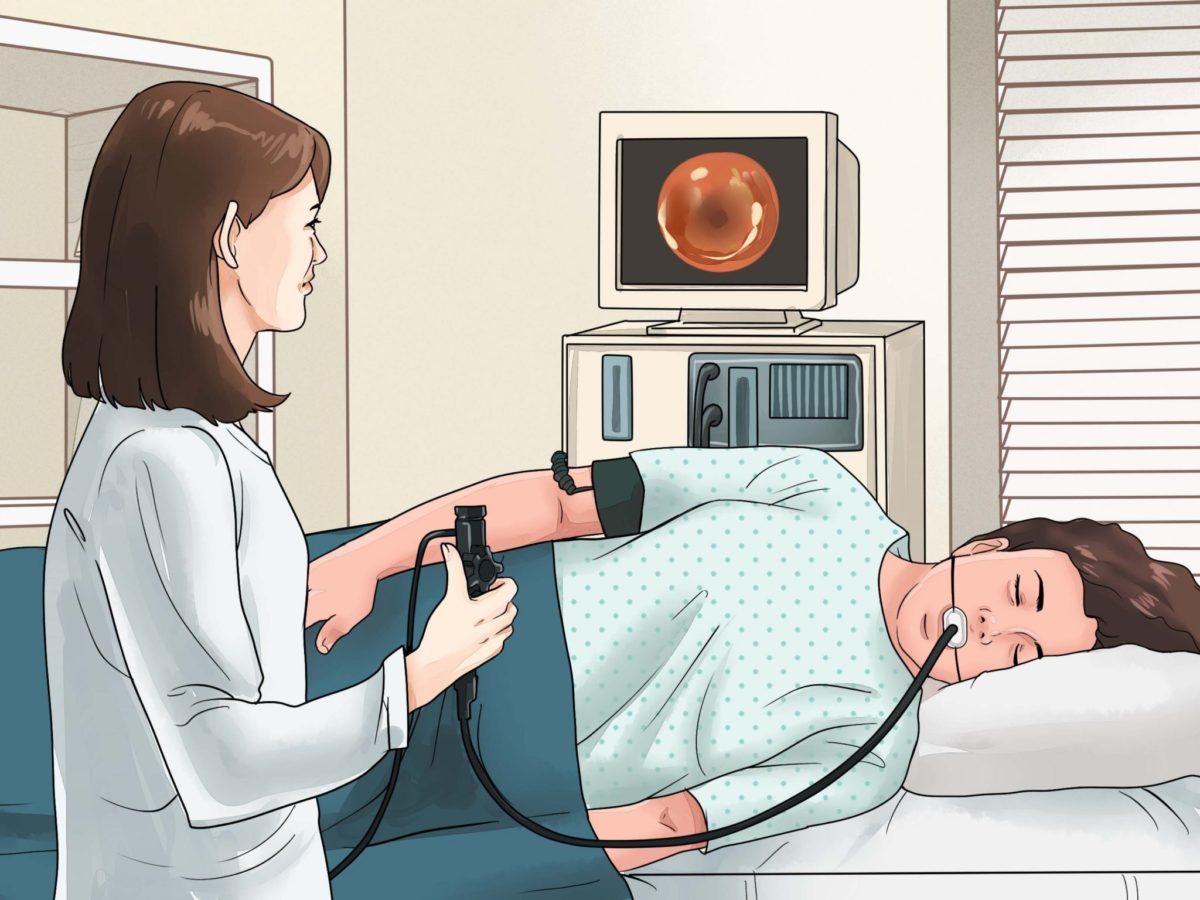
A gastroscopy usually reveals the diagnosis. It is an examination of the upper digestive tract (the esophagus, stomach, and duodenum) using a long, thin, flexible tube to view the internal lining of these organs
Treatment of PUD includes antibiotic medication to kill H pylori when it is present.
Drugs that inhibit stomach acid production, like proton pump inhibitors (PPIs), are given to promote healing. Examples of PPIs are omeprazole (Prilosec), lansoprazole (Prevacid), rabeprazole (Aciphex), esomeprazole (Nexium), and pantoprazole (Protonix).
Histamine (H-2) blockers also reduce the amount of stomach acid released and may reduce ulcer pain and promote healing. Examples are Tagamet (cimetidine), Zantac (ranitidine), Pepcid (famotidine), and Axid (nizatidine).
Antacids can provide rapid pain relief by neutralizing existing stomach acid. However, they are not considered useful enough to promote healing.
6. Gastroesophageal Reflux Disease (GERD)
Gastroesophageal reflux disease (GERD) is a common cause of epigastric pain.
GERD is a chronic digestive disease that occurs when stomach acid or stomach content flows back (reflux) into the esophagus.
Most healthy people experience acid reflux and heartburn once in a while. GERD should be suspected when these symptoms occur at least twice each week or interfere with daily life, .
The pain associated with GERD may be described as squeezing or burning. It may also radiate up to the chest, and sometimes to the back, neck, jaw, or arms.
Many people can manage the symptoms of GERD with lifestyle changes. Antacids are usually helpful too as they can neutralize gastric acid but the effects are usually short-lasting.
However, some patients may need prescription drugs, or even surgery, to reduce symptoms.
PPIs, H-2 blockers are commonly used to reduce symptoms.
7. Gastritis
Gastritis is an inflammation affecting the lining of the stomach.
Similar to gastric ulcers, it is sometimes caused by an underlying infection with the H pylori bacteria.
The symptoms include a gnawing or burning ache or pain in the epigastrium. Nausea and vomiting may also be present.
Common over-the-counter pain relievers, such as aspirin, ibuprofen (Advil, Motrin IB, others), and naproxen (Aleve, Anaprox) can cause gastritis. Stress and excessive alcohol consumption are also common underlying causes.
Medical treatment is essentially the same as that of peptic ulcer disease and GERD.
8. Pancreatitis
Pancreatitis is an inflammation of the pancreas. It can be both acute and chronic.
The main symptoms are upper abdominal pain, nausea, and vomiting.
The pain is characteristically dull, boring, and steady, and usually sudden in onset. It is most often located in the epigastrium and may radiate through to the back (9).
Gallstones and binge alcohol consumption are the most common underlying causes of acute pancreatitis.
9. Heart Attack and Acute Coronary Syndrome
Patients with imminent heart attack, also called acute coronary syndrome usually experience chest pain or tightness in the chest (10).
However, some patients may experience epigastric pain. There may even be a feeling of indigestion or fullness and gas.
10. Functional Dyspepsia
Functional dyspepsia is a chronic disorder that may cause discomfort in the epigastrium.
It is characterized by a feeling of fullness following a meal, early satiation, and epigastric pain (11).
The disorder is defined as functional because there are no observable or measurable structural abnormalities found to explain the symptoms. Hence, it is sometimes called non-ulcer dyspepsia as well.
Upper Left Abdominal Pain
11. Disorders of the Spleen
Upper left abdominal pain is sometimes caused by diseases of the spleen.
Enlargement of the spleen (splenomegaly) and splenic infarction may cause right upper abdominal pain (12).
Splenic infarction is a condition in which blood flow supply to the spleen is compromised.
Lower Abdominal Pain
Lower abdominal pain in women is frequently caused by disorders of the internal female reproductive organs. These disorders are not covered here.
12. Kidney Stones (Urolithiasis)
Kidney stones can be both small and large. Some stones stay in the kidney and do not cause any symptoms.
Sometimes, a kidney stone travels down the ureter, the tube between the kidney and the bladder. If the stone reaches the bladder, it can be passed out of the body in urine.
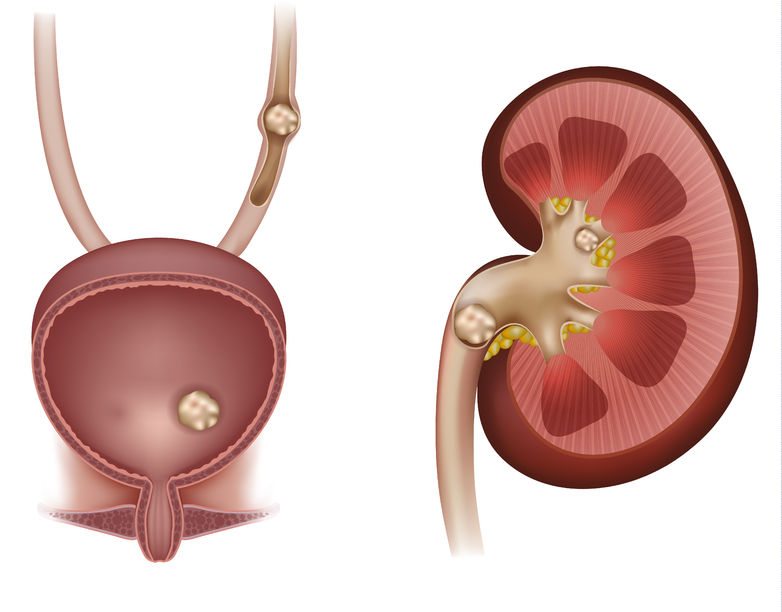
If the stone becomes lodged in the ureter, it may block the urine flow from that kidney. This may cause very serious and intense pain.
The pain is usually a sharp, cramping pain in the back and side, often radiating to the lower abdomen and groin. The pain often starts suddenly and comes in waves.
Nausea and vomiting may be present as well.
In addition, the urine may be dark or red due to blood (hematuria).
13. Cystitis
Cystitis is an inflammation of the urinary bladder. It is usually caused by a bacterial infection.
Cystitis may cause pain in the lower mid-portion of the abdomen.
There may also be a persistent urge to pass urine and a burning sensation while urinating.
Furthermore, blood in the urine (hematuria) may be present and sometimes the urine is cloudy and has a strong smell.
Bacterial cystitis is usually treated with antibiotics
14. Pyelonephritis
Pyelonephritis is a urinary tract infection that often begins in the urine bladder and travels up to one or both kidneys.
The symptoms include fever, chills, pain in the back or side of the abdomen, or the groin. Frequent urination, nausea, and vomiting are also common.
The infection is usually caused by bacteria. Hence, antibiotics are the first line of treatment.
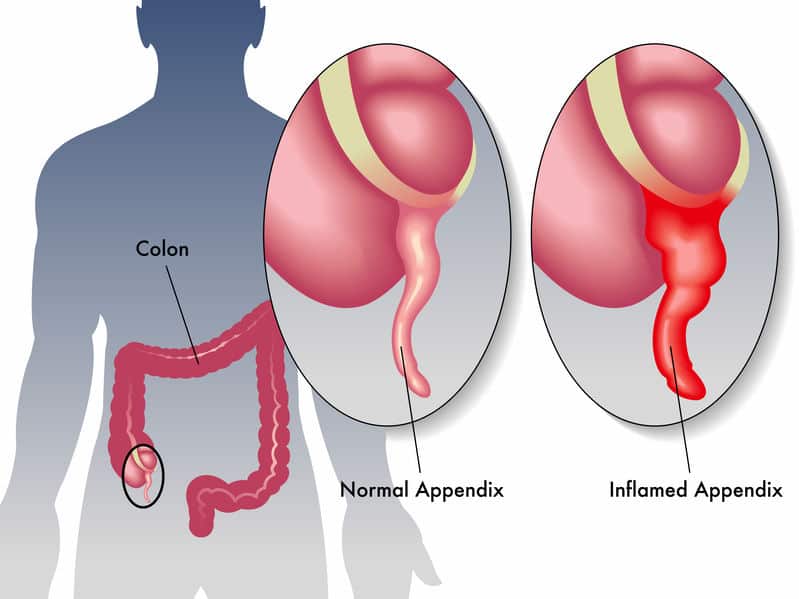
15. Acute Appendicitis
The appendix is a narrow, finger-shaped pouch that projects out from the colon
Acute appendicitis is an acute inflammation of the appendix and typically presents with pain around the navel. Usually, the pain radiates to the right lower quadrant of the abdomen.
The pain may increase with coughing, walking, or jolting movements.
Nausea and vomiting may be present, and there is usually a lack of appetite.
Acute appendicitis is usually treated by removing the appendix by open surgery or less-invasive keyhole surgery (laparoscopy) (20).
16. Diverticulitis
Diverticula are small, bulging pouches that can form in the internal lining of the colon.
Diverticulitis is defined as an inflammation of one or more of these pouches.
The symptoms include left lower abdominal pain, nausea, vomiting, and fever. Constipation, or less commonly, diarrhea may also be present.
Treatment usually includes antibiotics drugs.
Surgery is rarely needed unless complications are present.
Diffuse Abdominal Pain
Abdominal pain may often be diffuse and not located in a particular part of the abdomen.
17. Inflammatory Bowel Disease (IBD)
Inflammatory bowel disease (IBD) is a disease of a-unknown cause. It is believed to reflect an abnormal immune response to the intestinal microflora. Hence, it is classified as an autoimmune disease.
There are two major types of IBD, ulcerative colitis and Crohn’s disease.
Ulcerative colitis is limited to the colon whereas Crohn’s disease can affect any segment of the intestine.
The symptoms include abdominal pain and cramping, irregular bowel habits, and a passage of mucus with blood. Also, many patients experience weight loss, joint pain (arthralgia), sweats, and fatigue.
18. Intestinal Obstruction
Intestinal obstruction is a blockage that keeps food or liquid from passing through the small or large intestine.
There may be several underlying causes. Sometimes bands of tissue (adhesions) form in the abdomen after surgery. Cancer of the small or large bowel may also cause obstruction.
The symptoms include a crampy abdominal pain that comes and goes in waves. Besides, there is a loss of appetite, swelling of the abdomen, vomiting, and inability to have a bowel movement or pass gas.
Treatment depends on the underlying cause.
19. Gastroenteritis
Viral gastroenteritis, sometimes called stomach flu, is an infection of the small or large intestine.
Symptoms include watery diarrhea, abdominal cramps, nausea, vomiting, and sometimes fever (13).
Usually, symptoms only last a day or two.
Bacterial gastroenteritis is usually caused by consuming food that is contaminated with bacteria. Typical examples include Campylobacter and Salmonella.
Because gastroenteritis is usually self-limited, medical care is primarily supportive. Drinking fluid (oral hydration) is important. However, sometimes, intravenous fluids may have to be administered.
Antibiotics are administered for some cases of bacterial gastroenteritis (14).
20. Mesenteric Ischemia
The mesentery is a fold of membrane that attaches the intestine to the abdominal wall and holds it in place (15).
Acute mesenteric ischemia is caused by inadequate blood flow through the mesenteric vessels. It is a potentially life-threatening condition.
The condition is characterized by severe abdominal pain, sometimes associated with bloody diarrhea.
Acute mesenteric ischemia must be treated immediately to prevent tissue death. Surgery may be necessary to remove parts of the intestine.
21. Cancer
Several cancers may be associated with abdominal pain. Examples are cancer of the stomach, the liver, the pancreas, the colon, and the rectum.
22. Irritable Bowel Syndrome (IBS)
Irritable bowel syndrome (IBS) describes a group of symptoms that affect the large intestine without a known cause.
IBS is a common disorder and occurs more often in women than in men.
Symptoms of IBS include cramping, abdominal pain, and bloating. Diarrhea or constipation may be present as well.
Before the diagnosis is made, other more serious underlying causes of the patient’s symptoms should be excluded.


IBS has finally stopped being my painful companion as long as I remain on a grain free and low FODMAP diet. I was diagnosed 20 years ago.
Please don’t discount FODMAPS as the cause as it. It has a fair amount of science behinds it.
FODMAPs include fructose (when in excess of glucose), fructans, galacto-oligosaccharides (GO), lactose and polyols (eg. sorbitol and mannitol).
More information from the Monash University, Melbourne, Australia here: https://www.monash.edu/medicine/ccs/gastroenterology/fodmap
I may be part of the 10% you mentioned who needs surgery to address the life-threatening cause of my belly pain. We were told that I need to be operated on soon to remove stones from my kidney but I’m hoping that there are other options. It might be better to seek a second opinion online to see if I can find another type of treatment that might cure me.
I have had right upper quadrant pain for over a year. I recently had an endoscopy. The gastroenterologist found several things like a small hiatal hernia, esophagitis, GERD, biopsy revealed Barret’s Esophagus with pre cancerous cells and sensitivity to gluten. None of which explain my pain. I had my gallbladder removed over a year ad a half. Just had another MRI done and it revealed a Small fat signal lesion in the right side of the L5 vertebral body is compatible with a hemangioma of bone. That diagnosis still doesn’t explain my pain. Just another thing to worry about. I do have a small parapelvic (kidney) cyst that is considered small. It measures 1.1 cm. Could that be the cause of my constant pain, sometimes it’s a stabbing pain and I also feel it on my back.