Estimated reading time: 9 minutes
During the first few months of this year, we’ve seen at least three strong signs suggesting that health authorities have misled the public for several decades about dietary fats. This finding is of particular interest because later this year the 2015 Dietary Guidelines for Americans will be published.
Ever since the beginning of the 1960s, “eat less fat, in particular, less saturated fat and cholesterol” has been repeatedly emphasized by medical professionals and other experts.
Food manufacturers have played along by emphasizing low-fat food varieties of all possible kinds, whether it’s dairy products or something else. Butter consumption has decreased, and cooking oils have become very popular, all according to public health advice with the aim to eliminate cholesterol and saturated fat from our dishes.
What started all this was observational data showing an association between blood cholesterol and the risk of cardiovascular disease. Many health experts assumed that by reducing cholesterol and saturated fat in our diet the epidemic of heart disease might be stopped because these interventions would lower blood cholesterol. However, this was an untested hypothesis.
Nobody knew what would happen after the first US dietary recommendations were launched in 1980 because the implications of such an advice had never been tested in a scientific study.
Today, these guidelines may be regarded as a research protocol for the biggest dietary intervention trial so far performed. The trial was designed without a control group; everybody had the same advice. There was no informed consent and the trial wasn’t performed according to defined ethical principles for medical research involving human subjects (1).
However, to be fair, the death rated from coronary heart disease has dropped dramatically in most western countries for the past 30 years. Of course, this achievement is due both to modification of risk factors and improved treatment. Data from the US and many other countries suggest that lowering of cholesterol in the population may have contributed to this benefit (2).
On the other hand, since the introduction of the dietary guidelines, rates of obesity and diabetes have risen dramatically.
In fact, questions have repeatedly been asked about the Dietary Guidelines for Americans. It has been pointed out that the guidelines were implemented despite lack of supportive evidence and in the face of contradictory evidence (3).
Recently, the Dietary Guidelines Advisory Committee published its Scientific Report (4) preparing for the upcoming 2015 edition of the Dietary Guidelines for Americans. The U.S. Department of Health and Human Services (HHS) and the U.S. Department of Agriculture (USDA) jointly publish the Dietary Guidelines every five years.
The Scientific Report reflects important changes regarding dietary fats compared with previous guidelines. At the same time, two recent scientific publications suggest that our basic assumptions on dietary fats may have been wrong from the beginning.
Dietary Cholesterol
Recommendations to reduce dietary cholesterol were initiated by the American Heart Association (AHA) in the 1960s and have been a mainstay of the USDA and other public health guidelines for many years. All this time, excess dietary cholesterol has been regarded as a public health concern.
According to the Recent Scientific Report from the Dietary Guidelines Advisory Committee (4), ”Cholesterol is not considered a nutrient of concern for overconsumption.” It is assumed that this change of direction will make it to the final guidelines that will be published later this year.
Although blood levels of cholesterol are still considered an important risk factor for cardiovascular disease, the abrupt change of direction reflects scientific data suggesting that cholesterol consumed in food appears to play a minor role in determining the blood levels of this substance.
So apparently, the guidelines have been wrong for decades. There is no reason anymore to believe that eating eggs or other food rich in cholesterol will cause heart disease.
It will be interesting to see how the AHA will approach this recent change of heart.
Saturated Fat and Heart Disease
From the beginning, dietary guidelines have underscored the importance of limiting the amount of saturated fat in our diet. This advice was based on observational data showing an association between the intake of saturated fats and death rate from heart disease.
It is well known that although observational studies may show an association between two variables, they can very rarely prove a causative relationship. Although dietary guideline committees have always been aware of this fact, they have been determined to stick with their initial approach regarding saturated fat, most likely because of their immense respect for blood levels of LDL cholesterol (5).
For decades, LDL cholesterol has been regarded as an important target when it comes to reducing the risk of heart disease. It’s often assumed the almost every measure able to lower LDL cholesterol will be beneficial.
There is some evidence linking the consumption of some types of saturated fat with raised LDL cholesterol. Accordingly, these fats will increase risk. But, using surrogate markers like LDL cholesterol to determine risk may be misleading (6).
Only randomized clinical trials can prove that the intake of saturated fats will increase the risk of heart disease. Interestingly, results from such trials were available the time of the publication of the first dietary guidelines
Last month, British investigators published a systematic review and meta-analysis of results from randomized clinical trials that were available when the first US and UK dietary guidelines were published in the late 1970s and early 1980s (7).
The authors found six dietary trials, including a total of 2.467 male participants. The intervention differed somewhat between studies but all aimed at reducing total fat and/or saturated fat consumption in the intervention group.
There were no differences in all-cause mortality and non-significant differences in mortality from heart disease, resulting from the dietary interventions. The reductions in mean serum cholesterol levels were significantly higher in the intervention groups.
So despite lowering cholesterol, interventions aimed at reducing saturated fat intake did not lower mortality nor decrease death rate from heart disease.
The authors arrived at three pretty sobering conclusions:
Government dietary fat recommendations were untested in any trial prior to being introduced
Dietary recommendations were introduced for 220 million US and 56 million UK citizens by 1983, in the absence of supporting evidence from randomized clinical trials
The present review concludes that dietary advice not merely needs review; it should not have been introduced
Macronutrient Consumption Data
In 1977 the U.S. Senate Selection Committee on Nutrition and Human Needs issued Dietary Goals for the United States, which recommends that fat consumption be reduced to 30% of energy intake, and that carbohydrate consumption be increased to account for 55-60% of energy intake (8).
The focus on the relative contribution of different macronutrients was maintained by the first Dietary Guidelines for Americans that were launched by the USDA in 1980 and have remained largely unchanged since then.
There were two reasons experts believed reducing fats and increasing carbohydrates would be beneficial. Firstly, this would lower blood cholesterol and thereby the risk of heart disease. Secondly, because one gram of fat contains more calories than one gram of carbohydrates, the intervention would reduce the risk of obesity.
A recently published U.S. paper addresses the long-term dietary consumption of the U.S. population from 1965-2011 based on NHANES (National Health and Nutrition Examination Survey) data focusing on Americans aged 18-64 (9).
The main goal of the study was to address whether Americans have been following dietary guidelines with regards to the macronutrient composition of the diet.
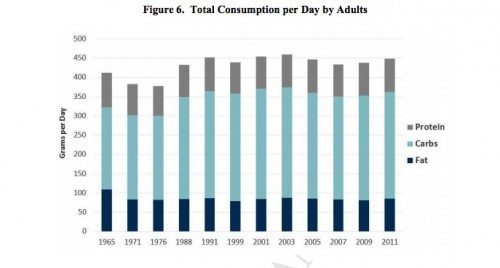
In 1965, fat consumption comprised 44.7% of calories of adult Americans’ diets, compared with 39% for carbohydrate. By 1999, fat consumption reached a through of 32.4% while carbohydrate consumption hit its peak at 52.1%. Protein consumption remained relatively constant throughout the period.
In 1971, saturated fat comprised 13.5% of total calories. By 2011, Americans were eating 10.7% of their calories as saturated fat (a 20.5% reduction since 1971).
Per capita cholesterol consumption decreased down below 300 mg/day, from over 400 mg/day in 1971.
The study also confirms a clear shift towards more obesity during the study period.
The authors underscore that there is a strong correlation between the increase in carbohydrate share of total intake and obesity.
They also address the question whether the increased prevalence of obesity can be explained by an increase in overall calorie intake by conducting their tests over two subsamples of participants who consumed similar calories over time. They conclude “the increase in calorie consumption since 1971 is not likely to offer any significant explanation for the increase in BMI (body mass index) over the last four decades.”
The main findings of the study were
- Americans have been adhering to federal dietary guidelines for the past 40 years
- Fat consumption by U.S. adults has decreased from 45% to 34% between 1965 and 2011
- Carbohydrate consumption has increased from 39% to 51% over this same period
- There is a high correlation between the change in diet and the rise of obesity
- The percentage of overweight adults has increased from 42% to 66% since 1971
The Bottom Line
Recently we have seen important evidence suggesting that the fear of dietary fats, in particular, the fear of saturated fats and cholesterol is not based on reliable scientific data.
This evidence adds further to the belief that we have been misinformed for decades by public authorities about dietary fat intake.
Although authors of dietary guidelines seem to have admitted that there is no reason to avoid dietary cholesterol, I’m still afraid they haven’t got it right. For example, the advice to avoid saturated fats was never based on evidence from randomized clinical trials.
It is hard to accept that public health recommendations are not based on solid scientific evidence.
A part of the problem is that the guideline process is too complicated, and recommendations are often hard to change.
The dietary fat history is a tragic example of how easy it is to mess things up for years when you get it wrong from the beginning.
Guideline writers should acknowledge the lack of evidence for most recommendations and write shorter guidelines. They should stick to hard evidence. Who needs hundreds of pages of expert consensus? The public deserves to be guided by real science.
Finally, despite the forthcoming 2015 Dietary Guidelines for Americans, this could be the year of the fat.



Good commentary. Indeed, the Dietary Guidelines Advisory Committee would do well to stick to hard science. There is no hard science linking saturated fat intakes to heart disease. There is hard science indicating that intakes of linoleic acid exceeding 2 percent of calories causes problems. For example, “Linoleic acid (LA) is the most abundant polyunsaturated fatty acid in human diets, a major component of human tissues, and the direct precursor to the bioactive oxidized LA metabolites (OXLAMs), 9- and 13 hydroxy-octadecadienoic acid (9- and 13-HODE) and 9- and 13-oxo-octadecadienoic acid (9- and 13-oxoODE). These four OXLAMs have been mechanistically linked to pathological conditions ranging from cardiovascular disease to chronic pain. Plasma OXLAMs, which are elevated in Alzheimer’s dementia and non-alcoholic steatohepatitis, have been proposed as biomarkers useful for indicating the presence and severity of both conditions. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3467319/
The Sceptical Nutritionist says, “About the only thing that all these seed oils have in common is that they are relatively low in saturated fat, which is considered to be a good thing by every reputable nutrition and heart health authority in the world. https://scepticalnutritionist.com.au/#sthash.45L4vrTy.dpuf
One wonders how much longer reputable scientists will be able to get away with ignoring all those lines of evidence suggesting it was a mistake to substitute seed oils for traditional fats. https://bit.ly/1Lz6CKA
Dear Dr. Sigurdsson,
I’d greatly appreciate a reference to my work in your post. These ideas are nearly all derived from my work, including my recent op-eds in the New York Times and the Wall Street Journal, as well as my book, The Big Fat Surprise.
Thank you very much!
Nina Teicholz
Dear Nina
As you know I’ve read your book and respect your writing and research.
I’ve previously mentioned your book on my blog in the context of dietary fats and will be happy to do so again. It so happens that I’ve been writing blog articles about dietary fats for some years now, starting long before your book was published. I don’t think you’ve referred to any of my writings.
The three issues/studies I bring up in this particular blog article are based on my own studies and opinion. The fact that some of my writing may coincide with your opinion doesn’t mean that “these ideas are nearly all derived from your work”.
As a clinical cardiologist for more than 20 years, blogger and author of academic papers I might have an angle/opinion to share.
“… respect your writing and research.”
WTF? Why? Do yourself a favour and check out these
https://thescienceofnutrition.wordpress.com/2014/08/10/the-big-fat-surprise-a-critical-review-part-1/
https://thescienceofnutrition.wordpress.com/2014/06/30/the-big-fat-surprise-a-critical-review-part-2/
And how many of the ideas in your book were derived from GCBC by Gary Taubes?
Are we supposed to bow down to the all knowing Nina Teicholz??
Research is research – live with it!
Mrs. Teicholz,
quite a few of us readers, just like Dr. Sigurdsson, are trained medical doctors with primary knowledge and sometimes primary research in the matter, and as much I’m sure your book (which I haven’t and will not read) is a wonderful compilation by a non-technical bright popularizer, please rest assured that most of us build our medical knowledge from trusted peer reviewed articles and not the last greatest book or personal hypothesis we’ve read about. So maybe there’s some sense lost in translation (I am not an English mothertongue speaker) but to me your statement sounds like a shameless self-promotion which would probably be more productive elsewhere.
This is great. Thanks for stepping down from your pedestal to share your opinion. I found Ms. Teicholz’s work far more informative than anything here, which is amazing considering she doesn’t have your privileged education.
I was gonna let this one slide but what the heck…
Robert – you’re kidding yourself if you think that “peer review” means diddly squat when it comes to the correctness of a study. The abuses of peer review are shameless in many fields, nutrition and climatology spring to mind as supreme examples.
Having actually read The Big Fat Surprise I feel like I can make an educated comment about it – it’s a terrific expose of just how poor nutritional guidelines are that delves not into just the science and history but also the personalities, which is quite important. I would suggest you read the book and then see if you still feel like making uncomplimentary remarks to the author.
@Robert
https://carbsanity.blogspot.com/2014/05/no-big-surprise.html
https://carbsanity.blogspot.com/2015/02/nina-teicholz-corrects-big-fat-surprise.html
Perhaps the point is that Big Fat Surprise had a major influence on the attitudes to fat in mainstream media that are an important part of the subject being discussed, not that Axel has necessarily used any of Ms Teicholz’s intellectual property in this post.
Hi re the cholesteroland dietary fat esp saturated fat what do you suggest if someone has high lpa and should reduce unsaturated fat and carbs but increase saturated fat ..BUT has the apoe 3/4 gene which calls for very very low fat from all sources..little to no saturated at all little to no animal protein and high carb and low to NO cholesterol as apoe4 s over absorb cholesterol and fat from the food we eat ..im a rock stuck in a hard place
“In 1965, fat consumption comprised 44.7% of calories of adult Americans’ diets, compared with 39% for carbohydrate. By 1999, fat consumption reached a through of 32.4% while carbohydrate consumption hit its peak at 52.1%. Protein consumption remained relatively constant throughout the period.
In 1971, saturated fat comprised 13.5% of total calories. By 2011, Americans were eating 10.7% of their calories as saturated fat (a 20.5% reduction since 1971).”
If total calories increased then the percentage increase/decrease would be affected by that and people are just playing around with numbers to prove a point.
Indeed. Carbsane appropriately demolishes this nonsense – which Axel sadly seems to have swallowed just like that.
What puzzles me is that nobody on either side of the saturated fat divide pays attention to linoleic acid research.
“Linoleic acid (LA) is the most abundant polyunsaturated fatty acid in human diets, a major component of human tissues, and the direct precursor to the bioactive oxidized LA metabolites (OXLAMs), 9- and 13 hydroxy-octadecadienoic acid (9- and 13-HODE) and 9- and 13-oxo-octadecadienoic acid (9- and 13-oxoODE). These four OXLAMs have been mechanistically linked to pathological conditions ranging from cardiovascular disease to chronic pain.”
https://www.ncbi.nlm.nih.gov/pubmed/22959954
What bothers ME about that comment Dave is that it’s a strawman. Plain and simple.
You’ve been told before that normal consumption of n-6 fatty acids is by no means detrimental. You’ve paid no heed to this.
“You’ve been told before that normal consumption of n-6 fatty acids is by no means detrimental.”
That depends what you want to die of
https://www.ncbi.nlm.nih.gov/pubmed/16573374
I had gone over to the low carb crowd years ago, getting 70% of my cals from saturated fat, about 20 from protein and 5 or less from carbs. My total C went from 185 to 404, LDL from 105 to 305. All other numbers good. So, within the low carb crowd there are some that say whoa, that is too high and others who say, under 500 or 600 its still not a problem.
Hi Joe
It’s well known that eating much saturated fats raises total, LDL and HDL cholesterol. What this means in terms of risk is still a matter of debate.
We also have to keep in mind that not recommending a limitation of saturated fat intake is not the same thing as encouraging high intakes.
I’d like to understand more about the saturated fat and total cholesterol connection. Could you comment on my thinking that for a rise in TC to be attributable to saturated fat, the fatty acids would need to be extracted and fed separately. Otherwise, aren’t we observing what happens when foods are eaten and then attributing the effect to different components? Ancel Keys made up his equation by doing this, which led to the belief that sat fat raises chol, PUS reduces it and MUS is neutral. He deemed butter to be sat fat and the short term rise in TC in test subjects was attributed to it. I think it was Prof Reiser who pointed out that it equally could have been the chol content of the butter. What I haven’t been able to find is good evidence for the connection between sat fat and chol, either biochem pathways or using extracted fatty acids. Can you help please?
Hi Jennifer
This is a complex issue. Stephan Guyenet covers some of the literature nicely here.
Guyenet’s post has several problems in it.
1) If you want to know accurately about the role of nutrient X on lipid levels, you need to conduct a metabolic ward study. Period. Observational studies among free-living individuals are BY DEFAULT incapable of examining this – they of course have their uses (more of which below) – as it is simply impossible to get free-living individuals to comply & report accurately. Guyenet’s comment on the “poor quality” of such studies suggests that he hasn’t actually read the original papers or e.g. Mensink et al (2003) meta-analysis of such studies – otherwise he would have known that e.g. his comment “hydrogenated oils as safa confounds etc.” is rubbish as the differences between safa and trans fat get addressed in it. Or perhaps he may be trying to downplay the matter to the favour of his way of thinking? Anyway, he does relent & mentions that the studies do point out that safa indeed has effects on blood lipids. Nice to see that he isn’t THAT far gone … 🙂
2) However, he tries to further mess the issue by (more or less clearly) stating that the effect would “short term”. This is a claim which of course requires direct evidence – and there’s no evidence pointing to the fact that LDL receptor function would somehow recover after a certain period of time. If it did, it would be unreasonable to expect this effect to be limited to safa only – and in this case we wouldn’t have as much CHD as we do know (LDL levels would always be near to optimal, as people in general do not start their lives with hypercholesterolemia). Observational evidence cannot – once again, BY DEFAULT – show this, due to methodological issues.
More on the issue of fats and lipids:
https://jn.nutrition.org/content/135/9/2075.full
3) Observational data can therefore – at its best – show that the effects of safa consumption (without appropriate control for a variety of other issues) in the range found in the studies doesn’t seem to be detrimental per se. Which, of course, is a no-brainer: it’s not safa per se, but its possible replacement in diet which modulates CHD/CVD risk.
Of course, one should bear in mind that individual safas differ somewhat in their effects on lipids. Furthermore, as no one ingests pure fatty acids without the actual carriers (food), certain foods rich in safa still do not have as adverse an effect on lipids as would be expected, e.g. fermented cheese, for which there are several mechanisms.
As for Jennifer’s question: based on her article, it seems that there simply isn’t (nor will there be) evidence that would satisfy her request. E.g. this
“Could you comment on my thinking that for a rise in TC to be attributable to saturated fat, the fatty acids would need to be extracted and fed separately. Otherwise, aren’t we observing what happens when foods are eaten and then attributing the effect to different components?”
shows remarkable ignorance on the question of e.g. individual safas and carrier foods (which I commented upon, the fermented cheese part). Findings in met.ward studies clearly indicate what is to be expected on the basis of LDL receptor findings.
Findings from very low carb studies show that increased SFA can’t raise LDL if there’s little CHO in the diet in most subjects, in fact LDL usually drops a tiny bit.
Which begs the question, what are feeding studies really looking at?
And then, of course LDL is not a discrete entity, the way glucose is, say, or insulin. The putative atherogenicity of the LDL particle is modified by CHO.
@Joe
Have you had your LDL-P checked?
I would not bet against something along the lines of ‘Our recommendations remain just as correct as the day we coined them*, but because there may have been some increase in overall calorific consumption, we must do MORE of the same. We therefore now recommend a reduction in total fat intake to below 25% of total energy intake (SFA 5% or less) and that CHO be increased to a minimum of 60%.’ There might even be a mention in favour of PCSK9 cholesterol-lowering drugs.
*Note the cunning wording, allowing a get-out-of-jail-free play if ever required. (Cynical? Moi?)
And I meant to say thank you for another great article!
Hi Axel
Thank you for the link. I think Stephan may be saying the same thing; that Ancel Keys metabolic ward studies from the 60s are the basis of the sat fat/ chol connection. I’ll ask him though.
I’ve looked at those studies in some detail and the flaws are incredible. The Aust Heart Foundation admitted in a position paper that their dietary recommendations are based on Key’s work.
My paper was published last year and if you have time to have a look, I would really appreciate your opinion
https://dx.doi.org/10.4236/fns.2014.519201
Thank you, Jen
That’s interesting Jennifer.
Thanks for the link.
Repeating the low carb/cholesterol denialist mispresentation about Keys (which Seth, BTW, has addressed here),
https://thescienceofnutrition.wordpress.com/2014/04/21/fat-in-the-diet-and-mortality-from-heart-disease-a-plagiaristic-note/
misrepresenting the case of FH by cherrypicking one man’s opinion etc. etc. – and, in general, amusement that results from referring to select number of ancient papers as somehow being evidence showing that lipid hypothesis as we know it in 2014 would be fundamentally wrong.
What did you hope to accomplish with this, Jennifer?
To make people think, Mie.
People are still allowed to think, aren’t they?
Dr. Sigurdsson,
Thank you for keeping me up to date on the latest in regards to dietary fat and its causal relationship to disease-or, rather, non-relationship to disease.
I’m surprised the news media hasn’t picked this up in the states. I haven’t seen a single report on this on any of the news networks.
Could it have that little value?
So happy to have found your blog.
@ Jennifer Elliott, Around 1980 I read a book by Hal Huggins, DDS entitled “Why Raise Ugly Kids?” He recommended consuming 2 eggs and a quarter pound of butter to bring total cholesterol up if it was low and lower cholesterol if it was high. Charting cholesterol changes in patients who followed his advice, there was a convergence around 220 mg/dL. That value falls close to the lowest point of the cholesterol/ all cause mortality curve. https://healthcorrelator.blogspot.com/2009/12/total-cholesterol-and-cardiovascular.html
When asked how doing the same thing could produce different results, he noted that his advice always contained the recommendation to reduce sugar intake substantially. Note, reducing sugar intake would lower cholesterol and substituting butter for margarine and other polyunsaturated oils would cause cholesterol to rise. No mystery there.
Same principle operates with reduced carbohydrate intake. Oft times, people eating fewer carbohydrates reduce their total calorie intake but neither raise nor lower fat intake. Total cholesterol responds accordingly.
The year of the Fat…indeed! For me it’s a historic year since all my basic knowledge is shattered in pieces and now I wonder how I should raise my family!
Since I’m having heterozygous hypercholesterolemia type IIa and ApoE 3/4 allele I was teached all my life (and still am) that a carb-rich, low-fat diet should be my goal.
Now I’m testing for the 2nd time LCHF (lowCarb – high fat – the opposite!) and never had such fantastic LDL- and HDL-levels.
Even under statins (atorvastatin 40 mg) and ezetimibe LDL hardly made it unter 100 and now it has dropped to below 60 after 6 weeks LCHF with below 30 g carbs a day and approx. 70-80% of daily calories from fat!
I keep loosing all the additional weight and just feel great…
But my Doc keeps telling me that CRP will go up and inflammation may occour leading to artheroclerosis…but checking the literature, it tells me the opposite (https://www.ncbi.nlm.nih.gov/pubmed/24075505).
Who’s right?
The first time in my life I doubt the official advices and wonder how to raise my (also genetically burden) kid…still no butter? Or better leave the bread in the shelf?
Any advice?
Max
It’s weird that there’s no updated advice for guys like me. Heterozygous FH is said to be quite common – 1:500 and we’re leaving the field to all those drug companies selling statins and that’s it? Despite the fact that 80% of the tretated patients keep failing in reaching their recommended LDL?
I’ll need to figure it out by myself, I guess….
Max
Updated dietary advice based on …? FH cannot be managed by diet alone. Of course, when you lose weight your lipid levels improve, but that cannot go on forever. Surely you knew that?
I won’t doubt that I’ll need statins all my life long – that’s o.k.,
But guys like me are still told we should keep a carb-rich diet (60%) and reduce fat esspec. saturated fats.
But since I’ve tried LCHF my blood fats are better than ever and this effect can not be explained by weight loss alone (I’ve hardly lost any remarkable weight in 4 weeks). I wonder how much focus I should pay on this in educating my kid…sparing on the bread or on the butter, that’s the point!
Max
Max, What is the target LDL you are trying to achieve? It may be too low in view of this. https://www.eurekalert.org/pub_releases/2011-05/tau-cn050511.php
The target LDL – that’s a good point.
Our “official” recommendations are:
LDL-Cholesterol < 160 mg/dl (4,14 mmol/l)
That's no problem at all – since November 2013 I'm well below 100 and since I'm doing LCHF (lowCarb-highFat) I circle around 60 (with the help of 40 mg Atorvastatin and Ezetimibe).
Without Ezetimibe and a less potential statin (Simvastatin) I had 156-172 LDL cholesterol.
Before that, I used Cholestyramine only which caused a high variation of the LDL values (maybe a more dietary influence?) – between 100 and more than 400 but most of the time well above the recommended values.
I'm just surprised to learn that high fat diet doesn't influence LDL cholesterol (at least, under statins) but my Doc keeps warning that this doesn't mean anything – the saturated fats may cause inflammation and all that despite good LDL values.
Max
Max, I’ve studied the supposed connection between saturated fat and inflammation. The only connection is between serum saturated fats caused by high carbohydrate intake or saturated fats injected directly into the bloodstream or brain. Dietary saturated fat alone doesn’t promote inflammation. https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0113605
Not only is the Volek study problematic in terms of its methodology
https://carbsanity.blogspot.fi/2014/11/de-novo-lipogenesis-to-palmitoleic-acid.html
https://carbsanity.blogspot.fi/2014/12/that-new-volek-phinney-study-part-iii.html
https://nutrevolve.blogspot.fi/2014/11/carbs-sfas-and-circulating-fatty-acids.html
but palmitoleic acid isn’t “consistently associated” with adverse health outcomes. See e.g. Chowdhury et al (2014).
As far as inflammation is concerned, safa is about the same as average carbs. Pufa (n-3 in particular) is somewhat anti-inflammatory.
Chowdhury?
That the paper that’s too badly flawed and full of errors – until a low-fatter finds something in it to use?
Mie said, “but palmitoleic acid isn’t ‘consistently associated’ with adverse health outcomes. See e.g. Chowdhury et al (2014).
As far as inflammation is concerned, safa is about the same as average carbs.”
Need clarification. Palmitoleic acid is not a saturated fatty acid. What’s your point.
While I’m commenting, these two papers suggest that swapping linoleic acid for saturated fat is beneficial.
https://ajcn.nutrition.org/content/95/5/1003.full
https://diabetes.diabetesjournals.org/content/63/7/2222.full.pdf
By way of contrast:
https://medicalresearch.com/weight-research/genetically-modified-soybean-oil-plenish-only-slightly-healthier/12425/
“Need clarification. Palmitoleic acid is not a saturated fatty acid. What’s your point.”
Indeed it isn’t. But Volek et al. suggest that higher amount of palmitoleic acid associated with the high carb phase is the result of DNL – because of higher carb intake.
And yes, the two studies do indeed suggest the benefits of safa –> n-6 exchange.
@Mie
“So, to clarify your position, we are to accept this?
Swapping saturated fat and carbohydrates for linoleic acid – the main polyunsaturated fat found in vegetable oil, nuts, and seeds – lowers risk of coronary heart disease…”
https://www.hsph.harvard.edu/nutritionsource/2014/11/05/dietary-linoleic-acid-and-risk-of-coronary-heart-disease/
And ignore this because?
medicalresearch.com/weight-research/genetically-modified-soybean-oil-plenish-only-slightly-healthier/12425/
“And ignore this because?”
Because – and this applies to the gorilla study below too – animal studies on dietary fatty acids, carbs etc. etc. have little relevance in humans. To give just one example, consider carbs & DNL: paleonistas/low carbers love citing rat studies because DNL is of totally different magnitude in rats whereas in humans it’s virtually insignificant (therefore, eating carbs per se doesn’t make one fat). If soybean oil is bad for human consumption, it needs to be confirmed in studies conducted on humans.
@Mie
And how are gorillas like rats?
“If soybean oil is bad for human consumption, it needs to be confirmed in studies conducted on humans.”
Pregnancy
https://press.endocrine.org/doi/full/10.1210/jc.2012-2482
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3206402/
https://www.ncbi.nlm.nih.gov/pubmed/25172360
Heart health
Careful evaluation of recent evidence, however, suggests that allowing a health claim for vegetable oils rich in omega-6 linoleic acid but relatively poor in omega-3 α-linolenic acid may not be warranted
https://www.cmaj.ca/content/186/6/434.extract
Advice to specifically increase n-6 PUFA intake, based on mixed n-3/n-6 RCT data, is unlikely to provide the intended benefits, and may actually increase the risks of CHD and death. https://www.ncbi.nlm.nih.gov/pubmed/21118617
“…a number of important questions remain unanswered…few prior studies have evaluated both dietary and circulating PUFA biomarkers… very few studies have assessed how objective biomarkers of LA or AA relate to CVD risk… evidence for cardiovascular effects of alpha-linolenic acid (ALA), the plant-derived n-3 PUFA, and docosapentaenoic acid (DPA), a long-chain n-3 PUFA of metabolic origin, remains limited and inconclusive.
https://jaha.ahajournals.org/content/2/6/e000506.abstract
I find it peculiar that dietary advice to replace saturated fats with linoleic acid has persisted from 1961 to the present despite these uncertainties. Something is causing the rapid world-wide deterioration in the public health and it is not excessive saturated fat in conjunction with inadequate linoleic acid intake.
Conclusion: There are no human studies of the sort that would confirm the harm clearly seen from animal studies.
“And how are gorillas like rats?”
Because they’re both animals?
Then the others:
1) Cognitive skills: bear in mind the study designs (cross-sectional), notice the large n-3/n-6 ratios and the large amount of LA in general. Not to mention the dietary choices for linoleic acid, which usually tend NOT to be those recommended by e.g. the guidelines. A lot of variables.
N-3 fatty acids may indeed beneficial for cognition, yes – or rather their deficiency may be detrimental (as there’s little data to suggest the benefits of supplementation/higher dietary intake among people who already have a balanced, healthy diet). Or course, there are conflicting studies in this field as well, see e.g. de Groot et al, “Alpha-linolenic acid supplementation during human pregnancy does not effect cognitive functioning” (2014) on pregnant women.
2) Cardiovascular health: dealt with this already. I suggest you check out the earlier posts here. Until you do – and comment on them, instead of just copypasting new stuff – I see no reason to continue.
“Something is causing the rapid world-wide deterioration in the public health and it is not excessive saturated fat in conjunction with inadequate linoleic acid intake.”
No shit? Gee, I sure as hell didn’t know that e.g. the etiology of obesity or DM2 cannot be reduced to a single factor …
@ Mie
“the etiology of obesity or DM2 cannot be reduced to a single factor …”
I never implied that. I said, “Something is causing the rapid world-wide deterioration in the public health and it is not excessive saturated fat in conjunction with inadequate linoleic acid intake.”
The public health message is, “Swapping saturated fat and carbohydrates for linoleic acid – the main polyunsaturated fat found in vegetable oil, nuts, and seeds – lowers risk of coronary heart disease…”
https://www.hsph.harvard.edu/nutritionsource/2014/11/05/dietary-linoleic-acid-and-risk-of-coronary-heart-disease/
Do you agree with that or not? Humour me. Present the short version of your argument in response to this post. I honestly don’t recall anything you said that constitutes anything apprximating a powerful argument. And I don’t care to wade through all the previous comments you made in search of the relevant information. Thanks.
@ Dr. Sigurdsson,
Several times Mie has raised objections to my practice of including snippets of the articles I discuss and/or reference when I post comments. I do that by way of illustration so that readers don’t have to wade through entire articles trying to figure out what I was getting at. Also, opinions and data can be located and viewed in context. I like being able to do that when I read scientific papers. Do you or any other readers of this blog object to what I do? And if so, can you offer suggestions? Should I report on all information contained in scientific papers by paraphrasing or summarizing? And if so, how is that advantageous?
I get your point Dave. I don’t object. It’s a difficult road. I’m not in favour of much copy/pasting but if it’s clearly done in order to make a point I will accept it. Secondly, I prefer comments not to be too long, mostly because I believe very few people read lengthy comments. Then of course, it’s always better if you use your own words instead of someone else’s. But, I guess everybody has their style and I there’s no reason to let Mie dictate how you should do it.
Dave,
“Do you agree with that or not?”
The benefits of exchanging safa –> pufa? Yes, I do agree there are benefits.
“And I don’t care to wade through all the previous comments you made in search of the relevant information.”
That’s too bad. Perhaps you OUGHT to, however, instead of copy/pasting lengthy portions of various studies the methodology, focus etc. etc. of which is ALL OVER the place. If you see no point in trying, why should I repeat myself to you?
Your choice. Reply to my criticism or don’t. Whether we’ll continue on the topic is up to that.
Dave posts links to studies and you question the methodology, Then you post links to blogs.
I presume these are peer-reviewed blogs.
Quote: “For example, the advice to avoid saturated fats was never based on evidence from randomized clinical trials.”
First of all, there never were any advice to *avoid* saturated fats, as you know (since I presume you actually read the recommendations).
Second, regarding evidence from RCT’s. There are no RCT’s showing that trans fats directly increase risk for cardiovascular disease either. Would you say it’s unfair to recommend avoiding trans fats anyway? Similarly with added sugar etc. Since no RCTs have been done with hard endpoints, would you say that recommending a low sugar intake will be the next ” biggest dietary intervention trial so far performed” as well, and that we should ask for informed consent and ethical approval first? Or is it reasonable to have a double standard when it comes to saturated fat?
Erik
There was advice to “avoid too much” fat, saturated fat and cholesterol. When you’re informing patients like I do it practically means “avoid” because “too much” is obviously a matter of definition.
I accept your criticism regarding RCT’s. I know we often have to rely on observational data (smoking, trans-fats, added sugars etc). But that doesn’t mean we can ignore results from RCT’s when they’re available.
I know I’m a bit harsh calling the guidelines a research protocol. But, sometimes you have to stretch a bit beyond to be heard.
Maybe it’s emotional. As a cardiologist I have been advising people to stay away from saturated fats and cholesterol for years. I guess learning it doesn’t make much sense is like discovering that your wife’s been cheating on you for years without you having a clue.
Axel, if you instruct your patients with certain simple choices for food and/or ACTUAL diets, they more or less automatically get it right.
And as it has been commented multiple times here: if the RCT’s have failed to even test modification X properly, you CANNOT reason that the modification X doesn’t work per se. You can, of course, reason that recommending modification X has little value in clinical practice as it is, but that’s a different thing. If you were to follow the SAME short-sighted reasoning with dietary advice in general, you’d have to STOP recommending any kind of dietary interventions to people: they simply don’t work that well, according to RCT data. See e.g.
https://www.ncbi.nlm.nih.gov/pubmed/15824290
But of course you don’t. And you shouldn’t. And we all know (at least I hope) why.
Mie
Why would/should I recommend I dietary intervention that hasn’t been shown to work (like the one in the paper you cited)?
“But, sometimes you have to stretch a bit beyond to be heard.”
I’m afraid that in this case you’re not just “stretching”. You’re misrepresenting. Sadly, Erik’s points on the double standard don’t seem to be that far-fetched.
Mie (and Erik)
Mie wrote: “I’m afraid that in this case you’re not just “stretching”. You’re misrepresenting. Sadly, Erik’s points on the double standard don’t seem to be that far-fetched.”
Calling it double standard is fine with me if you prefer to make things personal. I guess I’m happy if my writing raises some eyebrows and makes people think.”
My purpose was to highlight the huge responsibility associated with providing lifestyle/dietary guidelines to millions of people. I’m sure we agree that such an advice should be based on very strong scientific data. If it’s based on a hypothesis, or an expert opinion, it can be regarded as an “intervention trial”.
Axel:
“Why would/should I recommend I dietary intervention that hasn’t been shown to work (like the one in the paper you cited)?”
That was for ALL dietary interventions.
If you were to rely on RCT data alone, you couldn’t really recommend anything but Med. diet (best results), could you?
What RCT evidence is being ignored?
You linked to the Nutrition article that shows that Americans have NOT altered diets in response to recommendations.
The meta-analysis paper (Evidence from randomised controlled trials did not support the introduction of dietary fat guidelines in 1977 and 1983: a systematic review and meta-analysis) suggests that results of available RCT’s were not taken into account when the first US and UK guidelines were launched.
The authors of the Nutrition article concluded that Americans HAVE altered diets isn response to recommendations. I assume you don’t agree 🙂
Axel, I suggest you read what Charles wrote above:
“If total calories increased then the percentage increase/decrease would be affected by that and people are just playing around with numbers to prove a point.”
Americans are now consuming more calories. The actual amount of e.g. fat hasn’t thus changed virtually at all.
Furthermore, when it comes to e.g. fat sources, intake of fruits and veggies etc. etc. Americans seem to be pretty far from guidelines.
Mie
I agree with that. I do realize that calories play a role.
This is a peer reviewed paper and all I did was summarize the findings and the authors’ main conclusions. These conclusions weren’t mine although I found them interesting (and bold I guess).
I don’t believe the obesity epidemic is only due to shift in relative contribution of macronutrients in the diet but it may have played some part as the authors suggest. Maybe recommending fats out and carbs in wasn’t that clever after all (which shouldn’t come as a surprise as it wasn’t supported by strong scientific evidence).
Axel, I’m afraid that this “I just copypasted it” argument doesn’t really cut it.
First of all, you of all people should know that CRITICAL examination of any study is essential (I’m referring to the error you spotted in that one study of which you blogged about).
Furthermore, why would you mention these in the context of making an argument about the alleged failure of guidelines UNLESS you yourself believed the conclusions needed to be taken at face value?
Defend your position if you can. If you can’t, change it. That’s how it should be. Both Charles and Erik, not to mention yours truly, have pointed out flaws in your reasoning (the “bottom line” part). What do you e.g. have to say in defense of “dietary fat history being is a tragic example” when you just attenuated your own position above? Where’s the DATA that indicates this? Or what’s the part where the guideline author don’t stick to “hard evidence”? The part where they don’t put all the money on a few RCT’s that have in many ways failed to study the very thing they were supposed to study? Or what is the “real science” that “the public” needs? Sensational claims made by several popular authors, claims which are (at best) cherry-picked and one-sided?
C’mon Axel, don’t let your standard slide like this.
Mie
I don’t have to “defend my position” I’m on the attack. All my arguments can be found in the above blog article.
I know you, Charles and Erik “have pointed at flaws in my reasoning”.
But I still have a few supporters.
My colleague, Steve Nissen at the Cleveland Clinic obviously shares my opinion. He’s renowned for his scientific thinking, and well I guess he’s quite “mainstream” as well. He, just like you and I, knows that CRITICAL examination of any study is essential. His words reflect the view of many other cardiologists today (as well as my own).
Let me quote a recent Los Angeles Times article:
“In recommending a reversal on cholesterol intake, the advisory panel has “moved gently in the right direction,” said Cleveland Clinic cardiologist Dr. Steven Nissen. Like much dietary advice given to Americans, strict limits on dietary cholesterol “were never supported by science,” he said.”
“Foreshadowing a debate likely to take place over the coming months, Nissen said the experts drafting the 2015 Dietary Guidelines should consider going further, reversing the guidelines’ long-standing designation of saturated fat as a “nutrient of concern for overconsumption.” Saturated fats increase blood cholesterol, and the same 2013 report from the American Heart Assn. and the American College of Cardiology that said limits on dietary cholesterol were unnecessary also made the case that there was no reason to curtail consumption of saturated fat.”
And on USA Today:
“It’s the right decision,” said Steven Nissen, chairman of cardiovascular medicine at the famed Cleveland Clinic. “We got the dietary guidelines wrong. They’ve been wrong for decades.”
“We told people not to eat eggs. It was never based on good science,” Nissen said.
Advice to avoid foods high in fat and cholesterol led many Americans to switch to foods high in sugar and carbohydrates, which often had more calories. “We got fatter and fatter,” Nissen says. “We got more and more diabetes.”
Recent studies even suggest that longtime advice on saturated fat and salt may be wrong, Nissen says.”
Axel, are you seriously resorting to argument from authority now? If Nissen has anything convincing to say on the matter, let him author a review or a new meta-analysis etc. to indicate e.g. that advice to avoid fat led to people eating more crappy carbs as part of SAD (Standard American Diet) – despite the fact that the QUALITY of the carbs was always a part of the recommendations! Opinions in popular press are irrelevant compared to peer reviewed work, regardless of who we’re talking about
Please. At least try, will you?
Regarding Harcombe’s metaanalysis, one important question is: Were these RCT’s fair tests of the recommendations or the lipid-hypothesis? Except the Sydney trial (which is difficult to extrapolate), none of the RCT’s tested a diet with maximally 30 % energy from fat and 10 % energy from saturated fat.
If the authors read the papers the cite, they should not have ignored this advice in ‘Which clinical studies provide the best evidence?’ https://www.bmj.com/content/321/7256/255:
“Limited randomised controlled trials need other forms of evidence to be appraised and considered.
… the weight given to each bit of evidence should be determined by a detailed appraisal of the characteristics of that evidence.”
“The focus on the relative contribution of different macronutrients was maintained by the first Dietary Guidelines for Americans that were launched by the USDA in 1980 and have remained largely unchanged since then.”
No, the 1980’s U.S. guidelines did not say anything about the proportion of fat. They said “Avoid too much”. However, in the Scandinavian countries, the first official advice to limt fat to 35% (to lower the energy density) came already in 1968.
Erik
Thanks for the clarification.
The U.S. Senate Selection Committee on Nutrition and Human Needs launched the macronutrient composition goals in their 1977 report; Dietary Goals for the United States.
And you’re right. It say’s “avoid too much” fat, saturated fat and cholesterol in the 1980 guidelines.
Teicholz’s Book is less than useless, riddled with mis-information and plagiarism.
Instead of giving it to an op-shop (where someone else could be misinformed) I binned it.
But all is not lost…..I learnt not to pay attention to ‘book reviews’
The ilk of this woman and her shameless self promotion is evident in her comment and insult to Axel.
Axel – excellent article. Thanks for your good work.
Great article. Amazing how easy it is for society to get lost in all the science and to forget that if we just eat real, quality, preferably ethic and organic produce from all food groups and home cooked from scratch, we will not have to think about macro or micro nutrients, but can just have a really good time over food with our families and friends…
Thanks Sissa
You make an interesting point. The macronutrient discussion is probably outdated. I agree it’s time to talk about food.
The Dietary Guidelines Advisory Committee says it nicely in its recent Scientific Report: “Additional strong evidence shows that it is not necessary to eliminate food groups or conform to a single dietary pattern to achieve healthy dietary patterns. Rather, individuals can combine foods in a variety of flexible ways to achieve healthy dietary patterns, and these strategies should be tailored to meet the individual’s health needs, dietary preferences and cultural traditions.”
Indeed. Focus should be on diets as a whole. Not to mention on HOW to improve people’s compliance.
This – inevitably, in my opinion – requires state-level interventions on e.g. taxation and health care services. If it were just a matter of educating people, we’d have much less CVD, diabetes, obesity etc. etc.
Dr. Sigurdsson,
It’s interesting that linoleic acid (LA) is excluded from debate regarding the causes of obesity and heart disease. Why is there so little interest in LA research? It exists, it’s accessible, and it’s compelling. Have you read “The Modern Nutritional Diseases: and how to prevent them by Fred and Alice Ottoboni? In my opinion, it’s the definitive popular nutrition book on inflammation. https://www.amazon.com/The-Modern-Nutritional-Diseases-Prevent/dp/0915241056
Thanks Dave.
I agree.
LA is probably something we should be discussing more.
I’ve read a lot you have written about it.
I must admit I haven’t dug into the literature really. I guess I should.
I suggest you start with the Modern Nutritional Diseases. You can familiarize yourself with the Ottoboni’s work at this site: https://ketopia.com/author/ottoboni/
Will you consider studies like these too?
– Long-chain conversion of [13C]linoleic acid and α-linolenic acid in response to marked changes in their dietary intake in men
– Increasing dietary linoleic acid does not increase tissue arachidonic acid content in adults consuming Western-type diets: a systematic review
– Comparison of dietary conjugated linoleic acid with safflower oil on body composition in obese postmenopausal women with type 2 diabetes mellitus.
– Effects of n−6 PUFAs compared with SFAs on liver fat, lipoproteins, and inflammation in abdominal obesity: a randomized controlled trial
– Effect of dietary linoleic acid on markers of inflammation in healthy persons: a systematic review of randomized controlled trials.
– Overfeeding polyunsaturated and saturated fat causes distinct effects on liver and visceral fat accumulation in humans
😉
… or maybe you should write a guest article on the subject on Doc’s Opinion Erik and I’ll stick with Cardiology.
@Erik Arnesen,
I have collected all the studies you posted except this one – Long-chain conversion of [13C]linoleic acid and α-linolenic acid in response to marked changes in their dietary intake in men. Thanks. However, there are a number of aspects of LA research not addressed in the above papers. One example: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC41359/ Figure 3. “… the fractional PUFA content is the primary determinant of oxidation and PUFA compose 20% of total fatty acids in LDL.”
Mie says, “You’ve been told before that normal consumption of n-6 fatty acids is by no means detrimental. You’ve paid no heed to this.”
What is meant by normal consumption of n-6 fatty acids? Vague statement.
Were the gorillas in the Cleveland Zoo that developed heart disease on a diet that included 6.5% fat calories supplied by soybean oil not consuming enough n-6 to keep their arteries clear? https://www.marionzoological.com/leaf-eater/nutrition/
Or were they getting too much sugar? Or were they not getting enough fiber? Or was it the reverse; too much n-6, not enough sugar, and too much fiber? Whatever the case, it is clear manufactured foods containing soybean oil and sucrose can be problematic.
https://www.huffingtonpost.com/tana-amen/healthy-diet_b_2867253.html
Keith Ayoob says, “Polyunsaturated oils, mainly found in plant oils but especially high in sunflower, corn, and soybean oils, have all but gone off the populist radar. Chefs seldom speak of wild salmon drizzled with soybean oil or a salad with corn oil vinaigrette. Somehow, these don’t quite make the mouth water in the same way. Okay, fair game.
“But these liquid oils are loaded with polyunsaturated fatty acids, or PUFAs, and specifically loaded with a PUFA called linoleic acid, an omega-6 fatty acid that may deserve our renewed attention.
“In a recent meta-analysis (no reference so we don’t know how recent of which one) that focused on swapping out saturated fat for polyunsaturated fat — linoleic acid in particular — there was a strong and positive association with a combination of less saturated fat and more PUFA fat, as linoleic acid. The more linoleic acid consumed, the greater reduction in heart-related death and heart-disease events.” https://www.medpagetoday.com/PrimaryCare/DietNutrition/50326
But Christopher Ramsden (2010) says, “This detailed methodological evaluation of RCT found that mixed n-3/n-6 PUFA and n-6 specific PUFA diets have significantly different effects on risk of non-fatal MI þ CHD death. RCT that substituted mixed n-3/n-6 PUFA in place of TFA and SFA reduced CHD risk. By contrast, n-6 specific PUFA interventions tended to increase CHD risk. These increased CHD risks from n-6 specific PUFA diets may be underestimated as they replaced TFA and SFA; reductions of these potentially atherogenic fats would be expected to reduce CHD risk. Consistent with this, we found that the substitution of n-6 PUFA for TFA and SFA produced an increased risk of death from all causes that approached statistical significance, when analysed independently or in comparison to mixed n-3/n-6 PUFA diets. Among women, the only valid RCT that specifically increased n-6 PUFA found significant harm in the short term, and a signal toward harm with long-term consumption.” https://www.ncbi.nlm.nih.gov/pubmed/21118617
One reviewer remarked that there have been almost as many meta-analysis of RCTs involving saturated fats and omega-3s/6s as there are RCTs. As recently as December 2013 researchers were saying, “These recommendations are based on the beneficial effects of PUFAs on blood cholesterol and blood pressure, as well as epidemiologic and clinical trial evidence suggesting cardiovascular benefits of PUFA consumption. However, a number of important questions remain unanswered… few prior studies have evaluated both dietary and circulating PUFA biomarkers… recent randomized, controlled trials of fish oil supplements in high- risk patients have generally shown null results, raising concerns for true cardiovascular disease (CVD) benefits of n-3 PUFAs. In addition, whereas meta-analyses of prospective cohorts and of older clinical trials have seen lower CVD risk with higher consumption of n-6 PUFAs, largely linoleic acid (LA), concerns remain regarding the health risks of this PUFA, for example, because of concern that LA and its metabolite arachidonic acid (AA) may increase inflammation and thrombosis. Yet very few studies have assessed how objective biomarkers of LA or AA relate to CVD risk. Finally, evidence for cardiovascular effects of alpha-linolenic acid (ALA), the plant-derived n-3 PUFA, and docosapentaenoic acid (DPA), a long-chain n-3 PUFA of metabolic origin, remains limited and inconclusive.” https://jaha.ahajournals.org/content/2/6/e000506.abstract
So, with all this uncertainty, I’m supposed to accept what you tell me, “that normal consumption of n-6 fatty acids is by no means detrimental.”? I can’t do that. There’s too much evidence of harm with linoleic acid intakes exceeding 1 to 2% of calories.
Believe me, Mie. I will listen to anyone who furnishes convincing evidence that high intakes of linoleic acid are beneficial or, at the very least, benign.
https://ucrtoday.ucr.edu/27507
This just in. https://cbns.ucr.edu/faculty/sladek.html
1) Gorillas? WTF?
2) N-6 benefits: see e.g. the new Farvid et al (2014) on cohort data.
Or read the Ramsden et al (2010) which you mentioned: it showed that a) mixed n-3 & n-6 exchange was beneficial & the finding statistically significant whereas b) diets VERY rich in n-6 (consumption of 12-16% of tot.E as n-6) was worse but NOT in statistically significant way. Doesn’t lend any support to your pufa phobia.
3) And where’s the evidence of harm “with linoleic acid intakes exceeding 1 to 2% of calories”? Hmm?
Update: Responding to my request, Dr. Ayoob kindly sent me a link to the “recent” meta-analysis he referred to: https://circ.ahajournals.org/content/130/18/1568.abstract
From the abstract: “When the highest category was compared with the lowest category, dietary LA was associated with a 15% lower risk of CHD events and a 21% lower risk of CHD deaths.” Contrast this with the Lyon Diet Heart Study in which linoleic acid intake was substantially lowered with a resultant 70% drop in CVD morbidity and mortality. https://circ.ahajournals.org/content/99/6/733.full
Dave.
Can you give any explanation for the discrepancy between these studies. The Circulation meta-analysis suggests that replacing saturated fat with LA ma be beneficial in terms of CHD risk. I know it’s cohort studies, but it’s a large database. What do you think?
I am still studying this out. I’m about to request a Full Text of the Harvard meta-analysis Dr. Ayoob referred to in his commentary. https://circ.ahajournals.org/content/early/2014/08/26/CIRCULATIONAHA.114.010236.abstract
Here’s a thought. We know that heart disease mortality increased dramatically in the 1930s, 40s, and 50s and declined considerably beginning in the early 60s, coincident with a steep rise in lenoleic acid intake. (See Figure 6 in this article: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3076650/) The micronutrient and fatty profile of the food supply have undergone many changes through the years but the most striking change has been the increase in linoleic acid consumption.
It’s possible that increased linoleic acid intake may reduce CVD mortality when substituted for Saturated fats. But if it does so by shifting the cause of death to a variety of other fatal conditions related to the various effects noted in linoleic acid research literature, then that needs to come out in the analysis.
@DaveBrown9
Here’s the link to the full study
https://www.researchgate.net/profile/Maryam_Farvid2/publication/265093136_Dietary_Linoleic_Acid_and_Risk_of_Coronary_Heart_Disease_A_Systematic_Review_and_Meta-Analysis_of_Prospective_Cohort_Studies/links/54525ed70cf2cf51647a3448.pdf
“But if it does so by shifting the cause of death to a variety of other fatal conditions related to the various effects noted in linoleic acid research literature, then that needs to come out in the analysis.”
There’s no data to indicate that moderate intake of LA is harmful in the case of cancer: neither in RCTs (the old ones where the intake was, to put it mildly, sky-high) or in cohort studies.
So I’m curious: what are these “other fatal conditions” that you speak of?
@ Mie,
Linoleic acid (LA) is the most abundant polyunsaturated fatty acid in human diets, a major
component of human tissues, and the direct precursor to the bioactive oxidized LA metabolites (OXLAMs), 9- and 13 hydroxy-octadecadienoic acid (9- and 13-HODE) and 9- and 13-oxo- octadecadienoic acid (9- and 13-oxoODE). These four OXLAMs have been mechanistically linked to pathological conditions ranging from cardiovascular disease to chronic pain…lowering dietary LA can reduce the synthesis and/or accumulation of oxidized LA derivatives that
have been implicated in a variety of pathological conditions.” https://www.ncbi.nlm.nih.gov/pubmed/22959954
Regarding chronic pain:
“A dietary intervention increasing n-3 and reducing n-6 fatty acids reduced headache pain, altered antinociceptive lipid mediators, and improved quality-of-life in this population.” https://www.ncbi.nlm.nih.gov/pubmed/23886520
LA hard on veal calves:
Feeding tests were conducted to compare the feeding value of the following fats and oils for calves: butterfat, lard, tallow, coconut oil, peanut oil, corn oil, cottonseed oil and soybean oil. The effect of a very fat-poor diet on calves was also determined…In average daily gain in weight as well as in general well-being, the calves fed butterfat excelled those in all other groups. Following closely were those receiving lard and tallow. Corn oil, cottonseed oil and soybean oil were the least satisfactory. The average daily gains of calves in the latter three groups were .40 pound, .31 pound and .32 pound, respectively. They appeared unthrifty, listless and emaciated. Some calves in these groups died and others were saved only by changing to whole milk.
https://www.journalofdairyscience.org/article/S0022-0302%2842%2995274-3/abstract
@ Charles
Thanks for the link.
Dave, next time please just send the link/include the reference AND your own comments instead of needless, lengthy copy-paste.
First one
https://www.ncbi.nlm.nih.gov/pubmed/22959954
was about chronic headaches. Unfortunately, the study didn’t measure actual feelings of pain (unlike the other study) nor have a control group which would’ve resumed the regular diet with more n-6.
Second one
https://www.ncbi.nlm.nih.gov/pubmed/23886520
Unlike the first one, this study seemed to suggest particular benefit in increasing the n-3 intake (still, no control group with a regular diet, though).
Ok. Now please elaborate how big a problem chronic headpain is in terms of e.g. mortality or hospitalizations and then compare the benefits of moderate/higher LA intake in terms of of CVD/CHD. What is the benefit vs harm?
I’ll skip the calf study. Let’s keep the focus on people, shall we?
@Mie,
Aw Shucks! I like animal research. To me, ignoring what linoleic acid does to animals is like a crime scene investigator ignoring all evidence besides blood spatter and finger prints.
I especially like this 1973 research because for the first time, researchers demonstrated they could boost the linoleic content of meat and milk by protecting linoleic acid from microbial hydrogenation in the rumen with a protective casein-formaldehyde safflower oil coating. They also demonstrated that they could prevent the linoleic acid from killing the calves if it was protected with vitamin E. Too bad humans are never warned to boost their vitamin E intake to protect their metabolisme from the effects of high linoleic acid intake. https://www.animalsciencepublications.org/publications/jas/pdfs/37/6/JAN0370061419?search-result=1
I don’t understand the sudden change regarding dietary cholesterol and TC level.
As there been any new evidences that i’m not aware of? Because:
Dietary cholesterol and coronary heart disease.
”Confusion about dietary cholesterol has arisen because amounts above a certain quantity (the ceiling) do not elevate plasma cholesterol and low-density lipoprotein cholesterol. The therapeutic threshold for dietary cholesterol is below 100 mg/d.”
Dietary cholesterol from eggs increases the ratio of total cholesterol to high-density lipoprotein cholesterol in humans: a meta-analysis
”Dietary cholesterol raises the ratio of total to HDL cholesterol and, therefore, adversely affects the cholesterol profile. The advice to limit cholesterol intake by reducing consumption of eggs and other cholesterol-rich foods may therefore still be valid.”
Plasma lipid and lipoprotein responses to dietary fat and cholesterol: a meta-analysis
”Predictions indicated that compliance with current dietary recommendations (30% of energy from fat, < 10% from saturated fat, and < 300 mg cholesterol/d) will reduce plasma total and low-density-lipoprotein-cholesterol concentrations by approximately 5% compared with amounts associated with the average American diet.''
Effects of dietary cholesterol on serum cholesterol: a meta-analysis and review
''Serum cholesterol concentration is clearly increased by added
dietary cholesterol but the magnitude of predicted change is
modulated by baseline dietary cholesterol. T''
Also, plant positive did a review about did and found 19 studies which clearly show that dietary cholesterol increases TC level, as long as the TC level is low to beggin with, which is exactly what is being shown in all those reviews that i've put here.
https://www.youtube.com/watch?v=oWP-JDgAnvg&list=PLv3QDzdxan_IVgksyJDGR_PO6noKU0r_1&index=20
We can also look at this in reverse and see that vegan diet or any low-animal product diet clearly lower TC level.
There does not seem to be a new meta-analysis out about this so what are the new evidence that the comittee is talking about?
It seems pretty clear to me taht dietary cholesterol raises serum cholesterol and that the evidences are consistent.
And doctor, as a cardiologist, don't you think all these meta deserve your attention?
Frank. Here‘s a recent meta-analysis.
We have to look at clinical endpoints.
I don’t think there has been a study showing a significant association between intake of cholesterol rich food (like eggs) and the incidence or mortality from coronary heart disease.
Well, here’s one study
Egg Consumption and Risk of Heart Failure in the Physicians’ Health Study
and here’s another
Incident Heart Failure Is Associated with Lower Whole-Grain Intake and Greater High-Fat Dairy and Egg Intake in the Atherosclerosis Risk in Communities (ARIC) Study
also, the same years that the meta that you linked to was published, another one was, which came to a different conclusion.
Egg consumption and risk of cardiovascular diseases and diabetes: a meta-analysis.
”Our study suggests that there is a dose-response positive association between egg consumption and the risk of CVD and diabetes.”
Another one found no link for CHD for still a link for diabete
”Egg consumption in relation to risk of cardiovascular disease and diabetes: a systematic review and meta-analysis.”
Do you belive that diabete is not a risk factor for cardiovascular diseases? If you do, would you recommend a food that seems to promote diabete but still claims that it does not increases risk of CHD?
Also, eggs seems to promote certain types of cancer
Egg consumption is associated with increased risk of ovarian cancer: Evidence from a meta-analysis of observational studies.
Egg consumption and breast cancer risk: a meta-analysis.
As pointed out by Spences, serum cholesterol is not everything when considering CHD risk.
Dietary cholesterol and egg yolks: Not for patients at risk of vascular disease
”Diet is not just about fasting cholesterol; it is mainly about the postprandial effects of cholesterol, saturated fats, oxidative stress and inflammation. A misplaced focus on fasting lipids obscures three key issues. Dietary cholesterol increases the susceptibility of low-density lipoprotein to oxidation, increases postprandial lipemia and potentiates the adverse effects of dietary saturated fat. Dietary cholesterol, including egg yolks, is harmful to the arteries.”
And again, I think he summed it up nicely here :
”It is curious how Dr Fernandez, like many others, simply doesn’t want to look at the evidence. We summarized clearly the evidence that cholesterol has a permissive effect on, and amplifies the effect of, saturated fat. Dietary cholesterol clearly increases coronary risk. The same large, frequently cited studies that showed no harm from egg yolks among participants who remained healthy showed that egg yolks doubled coronary risk among participants who became diabetic during follow-up. The apparent absence of harm from egg yolks among people who remained healthy during the period of observation is probably an issue of statistical power.”
https://www.onlinecjc.ca/article/S0828-282X%2810%2900029-2/fulltext
I don’t think we can quickly jump to the conclusion, as you seem to do, that there is ”no reason anymore to believe that eating eggs or other food rich in cholesterol will cause heart disease”.
I believe there is quite strong reason to think that eggs and cholesterol rich food are unhealthy.
Frank, just like you quoted:
“Serum cholesterol concentration is clearly increased by added dietary cholesterol but the magnitude of predicted change is modulated by baseline dietary cholesterol”
The effect is not only considerably smaller when compared to safa or trans fat, but you also need to consider the sources (carrier foods). E.g. shellfish and eggs: rich in cholesterol, but also nutritious. Of course, if you have high LDL, you may want to choose foods that have a clearly beneficial effect. The overall picture is, nonetheless, still what counts.
In addition, it seems (based on the very reviews/meta-analyses you referred to) that egg consumption doesn’t really affect the general population but diabetics ought to be careful.
My understanding of this quote is that studying the effect of eggs consumption in a population with an already cholesterol-rich diet, with a high serum TC level is not likely to really show the arms associated with eggs consumption.
The effect could only be seen in people with low tc level and eating a plant-based diet. So it’s no surprise that it appears that eggs are harmless in the general population given that most american eat already too much cholesterol and have high serum cholesterol.
I also agree that we should consider the food as a whole. I’m not sure why you consider eggs nutritious; as a whole, they contains SFAs, cholesterol and choline, which seems to promote the formation of TMAO and could promote diseases.
What nutrients that is health promoting in eggs, that is hard to get elsewhere, that would outweigh these shortcoming? I’m not aware of any. My reasoning goes like this : if a food has clear disadvantage, and no real reason to be consumed, why would I consume it? I can get all the nutrition that I need from plants, without cholesterol, SFAs and choline, and i’m not missing out on anything. So to me the choice is quite obvious.
Out of curiosity, is by any chance you could be the same guy that used to called himself kismet on the longevity forum a few years ago? Your way of writing just makes me think of him. Doubt it tho’ cause as far as I remember, he was against eggs consumption 😉 Still curious!
“My understanding of this quote is that studying the effect of eggs consumption in a population with an already cholesterol-rich diet, with a high serum TC level is not likely to really show the arms associated with eggs consumption.”
But perhaps the consumption of eggs in met.ward studies conducted among vegetarians isn’t likely that show that either? We know that the human body can adjust cholesterol synthesis according to dietary intake of cholesterol. Now, doesn’t this mean that if the dietary intake of cholesterol is markedly higher for a period of time, the body will then ADAPT – resulting to lower cholesterol synthesis and lower tot.chol. levels in time? Or why else would the effect of dietary chol. on lipide levels be so modest on omnivores? 🙂
Notice that this is different with safa consumption, since there’s no data to suggest that LDL receptors are able to function better over time (otherwise there’d be MUCH less CHD/CVD).
“I’m not sure why you consider eggs nutritious; as a whole, they contains SFAs, cholesterol and choline, which seems to promote the formation of TMAO and could promote diseases.”
… and most of their fat is unsaturared, nice amount of different minerals, folate etc.
Of course, just like I stated, diabetics and people who need to actively lower their LDL significantly may of course be better off choosing something different.
“What nutrients that is health promoting in eggs, that is hard to get elsewhere, that would outweigh these shortcoming?”
Because it’s not a shortcoming in general population?
“Out of curiosity, is by any chance you could be the same guy that used to called himself kismet on the longevity forum a few years ago?”
Nope. I haven’t commented on his (?) forums. Had a clash with him here though a year or so ago. About eggs, BTW.
Replying here Mie as I can’t under your last reply.
”But perhaps the consumption of eggs in met.ward studies conducted among vegetarians isn’t likely that show that either?”
Strong designed studies (such as cross-over) have shown many times that dietary cholesterol do raise serum TC if baseline serum TC/dietary cholesterol are low enough. This is an harm to me, since I think the lipid hypothesis is well supported. Any food that increase TC level is not beneficial to me in this regard. No met ward studies could be long enough to study clinical endpoint such as CVD or mortality so i’m not sure how you think such studies could show more harm than we we already know.
”ow, doesn’t this mean that if the dietary intake of cholesterol is markedly higher for a period of time, the body will then ADAPT – resulting to lower cholesterol synthesis and lower tot.chol. levels in time? Or why else would the effect of dietary chol. on lipide levels be so modest on omnivores? :-)”
It might adapt – or not, see this (1) – but it adapts when it’s too late. We know TC should be under 150 mg/dl to be in the safe zone, but most americans are much higher than this. So if the body adapts, it does so too late, when the safe zone is already beyond. The studies shown in the plant positive video clearly show that when you have a below 150mg/dl, dietary cholesterol increases serum cholesterol to unhealthy range, where it might, or not, stabilize. At this point, studying the effect of one more egg per day is not likely to make any difference, hence when in the us population eggs appear harmless.
Also, as pointed out by Spences in the review i’ve mentionned above, baseline serum cholestrol in not everything. SAFAs and dietary cholesterol are pro-inflammatory in the post-prandial stage by themselves and harm the arteries. See the review for references.
”… and most of their fat is unsaturared, nice amount of different minerals, folate etc. ”
Again, what nutrient can’t I get elsewhere that I can get in eggs which also give me a fair amount of SFAs, cholesterol, and choline, which I don’t want? I get plenty of PUFAs from plants and i’m close to at least 1,5x RDAs for all of my vits and minerals. Why would I eat eggs?
”Because it’s not a shortcoming in general population? ”
Again, I believe that the us population is not a good reference as a population to study the harmful effect of different food, since their baseline diet is already pretty bad and their health in general also not optimal.
Based on the known effect of dietary fats and cholesterol, I think it it wise to avoid any food rich in SFAs and dietary cholesterol.
(1) See this video of Plant positive if you have not already, lots of good material in there. There a study where to author remarks that the idea that the body will stop producing cholesterol if dietary cholesterol is too high might not be true. Regardless, again, I think any food rich in SFAs and dietary cholesterol is best avoided.
https://plantpositive.com/pick-the-charlatan-nusi-guys-1/
“Strong designed studies (such as cross-over) have shown many times that dietary cholesterol do raise serum TC if baseline serum TC/dietary cholesterol are low enough.”
I’m not arguing against that, so why repeat it?
“It might adapt – or not, see this (1) – but it adapts when it’s too late.”
??? As these met. ward studies clearly show, if there’s baseline intake of any kind then the effect of added dietary cholesterol is clearly reduced – because the body indeed synthesizes LESS cholesterol if it gets more from the diet (this is not an opinion, you know). Now, this means that if the dietary intake remains up, then synthesis goes down
–> vegans will not have elevated plasma cholesterol long enough to get severe damage (atheromas take decades to build up). Otherwise EVERYONE in these studies would have elevated plasma cholesterol as no one starts with elevated chol. intake, right?
“Also, as pointed out by Spences in the review i’ve mentionned above, baseline serum cholestrol in not everything.”
I probably missed the review but here’s something from Spence et al.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2989358/
Ok, so postprandial inflammation etc. etc. are factors to consider too. However, notice that the takeaway message of the review is STILL to limit consumption if you’re a HIGH RISK individual. Not for each & every person. Furthermore, the evidence on factors besides lipid levels is still – in my opinion – somewhat secondary in high risk patients (you do know that the first and foremost intervention is to lower one’s LDL?), which of course means that the possible risk is further attenuated among those not of high risk.
”… and most of their fat is unsaturared, nice amount of different minerals, folate etc. ”
“Why would I eat eggs?”
You don’t have to. But you have no reason NOT to eat them in moderation as part of a normal, healthy diet. Think e.g. about whole grains: not quite as nutritious (when adjusted for tot. E) as veggies & berries, but does that make them a “no-no” as part of diet? Nope. A healthy diet isn’t a hardcore-don’t-eat-nothing-but-the-best kind of dogmatic diet.
“(1) See this video of Plant positive if you have not already, lots of good material in there.”
No videos for me, thank you very much. If you want, please link or give a reference to that study you mentioned in the final paragraph.
I’m keeping this going althought from reading your comments I know we agree on much more than we seem to disagree on, and I would probably not quite call this disagreement but just a matter of drawing a line somewhere in regard to our own standard.
”I’m not arguing against that, so why repeat it?”
I just repeated it because you said, in the other reply that ”Because it’s not a shortcoming in general population?”. My point is simply that any food that increase cholesterol, and that carries cholesterol, has and is a shortcoming to me when I consider what food I should eat to get the best odds of a good health.
”Ok, so postprandial inflammation etc. etc. are factors to consider too. However, notice that the takeaway message of the review is STILL to limit consumption if you’re a HIGH RISK individual.”
Well, again, my standard are higher, it seems. As pointed out in that same review from Spences
”Feeding of egg yolks induces inflammation characterized by elevations of C-reactive protein and serum amyloid A, but this effect is more pronounced in lean individuals without insulin resistance”
referencing this study
Cholesterol feeding increases C-reactive protein and serum amyloid A levels in lean insulin-sensitive subjects
there is also this study which found that the effect of dietary cholesterol is worst for IS individual
Effects of insulin resistance and obesity on lipoproteins and sensitivity to egg feeding
I’m lean and quite healthy according to my classic biomarker (TC 123mg/dl, low fasting glucose level) I clearly fall into the categories of individual for which eggs would seem to have a detrimental effect (raising my TC level and my inflammatory markers).
”You don’t have to. But you have no reason NOT to eat them in moderation as part of a normal, healthy diet. ”
Again, I might agree with you here for the general population, but i’m rather zealous when it comes to my health and I have no reason to consume a food that a) don’t bring me anything positive that I can’t get elsewhere and b) that brings me stuff that I can reasonnably think will have a negative impact on my health. For me a healthy diet is health promoting – anything that could raise my TC, LDL and inflammatory marker is not regarded as health promoting, for me.
It just a matter of where we draw the line I guess, as I said in the beginning.
The study was this one
Absorption, metabolism, and serum concentrations of cholesterol in vegetarians: effects of cholesterol feeding.
where the authors remark:
According to the current concept of cholesterol metabolism, enhanced absorption of cholesterol can reduce the synthesis of endogenous cholesterol, increase that of bile acids, and enhance the biliary reexcretion of cholesterol (1). In the vegetarians, however, the sterol balance data disclosed no significant decrease in cholesterol synthesis and serum cholesterol precursor sterols were actually unaffected by the
extra cholesterol intake, indicating that there was no lowering of
cholesterol synthesis. It is interesting that even very high longterm
cholesterol intake can impair fractional absorption of cholesterol
and enhance bile acid synthesis so that the synthesis of
cholesterol may be unchanged and serum cholesterol remains
normal (43).
So I don’t know. My point was only that it seems that cholesterol level stabilize once they are high. These studies clearly show that if you have low TC and dietary cholesterol intake, increasing dietary cholesterol intake will increase your TC level over 150mg/dl and then it might stop increasing, but that’s too high already in regard to athero plaques progression.
Again, I might simply draw the line a little bit more zealously when it comes to my health 🙂 and again, I know you are just going with a more balanced approach which I think is absolutly justified for the general population, and i’m not even saying that in the end it makes all that much of a big difference to eat a few eggs a week on a plant-based diet. I just don’t see any reasons to do it and don’t miss it.
Since you’re talking about eggs and cholesterol, I just found this paper that looks intriguing: “The influence of consuming an egg or an egg-yolk buttermilk drink for 12 wk on serum lipids, inflammation, and liver function markers in human volunteers.”
Quote from abstract: “The increase in serum TC and LDL-C concentration was no longer significant in women consuming the same egg yolk incorporated in a buttermilk drink (0.33 mmol/L [P = 0.66] and 0.31 mmol/L [P = 0.55], respectively).”
https://www.ncbi.nlm.nih.gov/pubmed/23911216
@ Frank, It may not be wise to rely on the opinions of Plant positive no matter how many studies he cites. For example, he says, “… the most basic assumption seems to be that it is an asset of saturated fats that they are resistant to oxidation. Don’t believe it. Actually, it is this resistance to oxidation along with its stiffer structure that makes saturated fat such a difficult thing for your body to deal with. If saturated fatty acids aren’t easily oxidized, that means they are not easily used for energy and other purposes. They tend to linger and cause trouble. The body treats them like foreign invaders.” https://plantpositive.com/41-pufas-oxidize/
There’s a big difference between oxidation of saturated fatty acids in mitochondria and auto-oxidation of polyunsaturated fatty acids cholesterol particles and elsewhere in the body. Excerpt: “Lowering dietary LA significantly reduced the abundance of plasma OXLAMs, and reduced the LA content of multiple circulating lipid fractions that may serve as precursor pools for endogenous OXLAM synthesis. These results show that lowering dietary LA can reduce the synthesis and/or accumulation of oxidized LA derivatives that have been implicated in a variety of pathological conditions.” https://www.ncbi.nlm.nih.gov/pubmed/22959954
I’m kind of perplex why you think that this quote from plant positive, and what you said next, discredit him.
I also don’t understand why you say that I should not listen to his opinion even if he cites studies. He just so happens to be citing studies that anyone with an internet connection can access for themselves and review, and they all clearly show that dietary cholesterol increases serum cholesterol.
@Frank
Even Ancel Keys said that dietary cholesterol had no effect on serum cholesterol.
Frank, I didn’t say you shouldn’t listen to plant positive’s opinion. I merely cautioned you to be careful about relying on his opinion. In truth, only the facts are reliable. When a person misrepresents the facts, his opinions should be regarded with suspicion.
This is the quote I referred to.
Also, plant positive did a review about did and found 19 studies which clearly show that dietary cholesterol increases TC level, as long as the TC level is low to beggin with, which is exactly what is being shown in all those reviews that i’ve put here.
https://www.docsopinion.com/2015/03/02/the-year-of-the-fat/#comment-19554
@Frank
https://circ.ahajournals.org/content/5/1/115.full.pdf
Human Atherosclerosis and the Diet
By ANCEL KEYS, PH.D.
In summary, then, we may remark that direct evidence on the effect of the diet on human atherosclerosis is very little and is likely to remain unsatisfactory for a long time. But such evidence as there is, plus valid inferences from indirect evidence, suggests that a substantial measure of control of the development of atherosclerosis in man may be achieved by control of the intake of calories and of all kinds of fats, with no special attention to the cholesterol intake. This means: (1) avoidance of obesity, with restriction of the body weight to about that considered standard for height at age 25; (2) avoidance of periodic gorging and even temporary large calorie excesses; (3) restriction of all fats to the point where the total extractable fats in the diet are not over about 25 to 30 per cent of the total calories; (4) disregard of cholesterol intake except, possibly, for a restriction to an intake less than 1 Gm. per week.
https://www.medscape.com/viewarticle/805580
Correlation Between Oxysterol Consumption and Heart Disease
The research conducted in my laboratory, as I described above, demonstrated that cholesterol is not a problem unless it is oxidized. Even Ancel Keys, who some consider the father of the cholesterol–heart disease hypothesis said in 1997: “There’s no connection whatsoever between the cholesterol in food and cholesterol in the blood. And we’ve known all along. Cholesterol in the diet doesn’t matter at all unless you happen to be a chicken or a rabbit”
https://ajcn.nutrition.org/content/32/5/1051.full.pdf
Effect of dietary egg on human serum cholesterol and triglycerides
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1245349/pdf/bmjcred00006-0011.pdf
Effect ofdietary cholesterol on plasma cholesterol concentration in subjects following reduced fat, high fibre diet
It seems Keys was mistaken on this issue. We have now plenty of evidence clearly showing that dietary cholesterol do raise serum cholesterol. See the multiples meta I’ve posted above.
” My point was only that it seems that cholesterol level stabilize once they are high. These studies clearly show that if you have low TC and dietary cholesterol intake, increasing dietary cholesterol intake will increase your TC level over 150mg/dl and then it might stop increasing, but that’s too high already in regard to athero plaques progression.”
I’m going in for new blood work in a couple of months and we shall see but my last blood work had TC 120, LDL-C 56, HDL-C 54
I eat meat and eggs among other things so is juts the stain I take or something else??
Hi Charles
Do you take statins or was that sarcastic? If you do that certainly must be influencinbg what’s going on.
There is clearly also genetical factors at play, maybe you have geneticaly low TC level and are not affected much by the food you eat.
Who knows. Good for you in any case. Those are very good numbers. Again, I think my prudent approach makes sens :
Avoid food that have clear downside, especially if they don’t have anything interesting to offer.
Eggs have been shown to increase TC level, LDL, Apo-b, inflammatory markers such as c-reactive p and serum amyloid a, are seemingly linked to CVD and some cancers in epi… and I can’t think of any nutrient that I should get from eggs that I can’t get elsewhere without those downsides. Again, we all choose where we draw the line. I’m not dogmatic about my stance, but based on my understanding of the science and my seriousness about my health, this is where I draw it.
@Frank
Last hsCRP was 0.9, fasting glucose was 83
https://carbsanity.blogspot.com/2015/03/not-really-surprised-nina-teicholz-digs.html#more
https://blogs.plos.org/dnascience/2015/03/05/man-ate-25-eggs-day/
The Man Who Ate 25 Eggs a Day
Fred Kern Jr., MD, a gastroenterologist at the University of Colorado School of Medicine, heard about the man and saw an opportunity to study individual differences in how diet affects serum cholesterol level. And so the 88-year-old egg eater joined such famous patients as French-Canadian explorer Alexis St. Martin and Henrietta Lacks.
First, Dr. Kern tested the man’s lipid levels, which were normal: 200 milligrams per deciliter total cholesterol and 142 for LDL. Then he compared the extent to which the man’s body compensated for the cholesterol overload in the 25 daily eggs to that of 11 volunteers who had their cholesterol tested under their usual eating habits and 16 to 18 days after adding five eggs a day. The Eggman was too obsessed to try to go without to help the study. Dr. Kern’s analysis, albeit limited, revealed a lot about how our bodies differ in what we do with lipids.
The 11 volunteers on average absorbed 54.6% of the dietary cholesterol while on their normal diets and 46.4% while on the egg diet. But the 88-year-old absorbed only 18% of his dietary cholesterol. Plus, his liver made less cholesterol than is common and shunted more of it into bile acids (which aid digestion) than did the livers of the volunteers, a metabolic triple whammy that Dr. Kern called “extremely efficient compensatory mechanisms.”
Basically the man’s metabolism adjusted to the overload in a way that kept his blood lipid levels both healthy and constant, the very definition of homeostasis. And he likely isn’t alone.
https://www.nejm.org/doi/full/10.1056/NEJM199103283241306
Normal Plasma Cholesterol in an 88-Year-Old Man Who Eats 25 Eggs a Day — Mechanisms of Adaptation
https://healthcorrelator.blogspot.com/2012/10/the-man-who-ate-25-eggs-per-day-what.html
The man who ate 25 eggs per day: What does this case really tell us?
This is what the study said verbatim:
https://www.nutritionjrnl.com/article/S0899-9007%2815%2900077-5/abstract
“Since 1971, the shift in macronutrient share from fat to carbohydrate is primarily due to an increase in absolute consumption of carbohydrate as opposed to a change in total fat consumption. General adherence to recommendations to reduce fat consumption has coincided with a substantial increase in obesity.”
So people are fatter now because they eat more, not because they decreased fat consumption. This article is misleading in this regard. Along with obesity comes a host of other related metabolic illnesses.
I’m curious why the billion Asians subsisting primarily on rice and vegetables didn’t get fat until they started adopting the rich western diet. From 1989-97, prevalence of overweight (BMI≥25) males in
China almost tripled. They were cruising along just fine until Burger King showed up.
Michael, Americans ended up swapping saturated fats for linoleic acid which has decidedly obesiogenic effects. Here’s what happened. “The incidence of obesity in the U.S. has increased from 15% to 35% in the last 40 years and is expected to rise to 42% by 2030. Paralleling this increase in obesity are a number of dietary changes, most pronounced of which is a >1000 fold increase in consumption of soybean oil from 0.01 to11.6 kg/yr/capita from 1909-1999: soybean oil consists of 50-60% linoleic acid (LA), so the energy intake from LA has increased from 2% to >7%/day. LA is an essential fatty acid and a precursor to arachidonic acid, which is linked to inflammation, a key player in obesity, diabetes, cancer, etc. Another component of the American diet that has increased substantially in the last four decades is fructose, primarily in the form of high fructose corn syrup in processed foods and sodas. The roles of both LA and fructose in the current obesity epidemic are under intense scrutiny but are not well understood and seldom compared side-by-side. https://press.endocrine.org/doi/abs/10.1210/endo-meetings.2013.OABA.9.SAT-708
Actually, LA is not under intense scrutiny except by a few researchers here and there. In fact, hardly anyone has ever heard of linoleic acid.
As for the rest of the World, people love their fried foods. In South Africa, for instance, ” A typical “low quality” meal consists of mostly mealie meal,
bread or rice, with very little animal protein or vegetables. The meal
is also usually prepared with cheap oil and lots of salt.” https://allafrica.com/stories/201504071317.html
In a 2003 Orlando Sentinel article entitled ‘Hunger Confronts Bigger Issue’, global obesity expert Barry Popkin repeatedly mentioned the global increase in the use of vegetable oils for food preparation:
“If you go back to those same villages or slum areas today … their diet includes a lot of vegetable oil … In China … Rice and flour intake is down, and animal-source foods such as pork and poultry and fish are way up, and the steepest increase is in the use of edible vegetable oils for cooking … People are eating more diverse and tasty meals; in fact, edible oil is a most-important ingredient in enhancing the texture and taste of dishes … The edible-oil increase is found throughout Asia and Africa and the Middle East as a major source of change.”
Note the increase in pork, poultry and fish. Same thing happened in the United States. Problem is, pork and poultry fat and meat contain considerable linoleic acid because, unlike ruminants, swine and poultry lack the where-with-all to biohydrogenate linoleic acid into fatty acids that would be more benign. Rather than furnish a link, I suggest anyone curious about biohydrogenation Google – “John Wallace biohydrogenation linoleic acid” and “Nancy Carol Baker Myristic Acid”.
From Baker’s Master’s Thesis: “Based on previous studies, we expected a significant relationship between levels of dietary linoleic acid and elaidic acid with levels of accumulation of each of these fatty acids in the plasma. Unexpectedly, there was not a significant relationship between the dietary and plasma levels of either of these fatty acids. In contrast, a significant correlation was found between dietary myristic acid, C14:0, and the plasma level for this fatty acid. The idea that dietary linoleic acid would predict for plasma linoleic acid was based on the fact that as an essential fatty acid, linoleic acid is not made in the body. Therefore, the plasma concentration of linoleic acid could depend on dietary consumption. Linoleic acid is plentiful in the American diet. Based on a 2000 kcal diet, linoleic acid consumption is estimated to be 6.7% of energy consumed (Harris et al., 2009). Since linoleic acid can be metabolized to long chain fatty acids, significant correlations to these fatty acids were considered probable but were not shown in this study
Myristic acid is considered the worst kind of saturated fat because it has the greatest impact on cholesterol levels. Yet Baker found that “The saturated fat, myristic acid, was inversely related to both trunk fat and total body fat…” Dairy products contain from 8 to 12% myristic acid. Perhaps this explains Ulrika Ericson”s recent findings. https://www.lunduniversity.lu.se/article/high-fat-dairy-products-linked-to-reduced-type-2-diabetes-risk
I don’t think it has to do with fatty acids, it has to do with the protein. High fat dairy is typically fermented, and the fermentation breaks down the proteins, which is why there is an associated reduction in type 2 diabetes. We see the same thing in the Masai tribe with their high consumption of fermented dairy and low consumption of meat.
Animal protein is the killer.
“I’m curious why the billion Asians subsisting primarily on rice and
vegetables didn’t get fat until they started adopting the rich western
diet.”
You changed the subject. You were wondering about the factors causing obesity, not cancer. Here’s more commentary that speaks to the obesity issue. https://www.doyoueven.com/2015/03/the-fat-that-makes-you-fat/
That’s an interesting article on LA. I’m not sure if it can explain the Chinese cancer and obesity explosion though. Perhaps a combination of LA and casein are at work.